Alison Dotson's Blog
February 13, 2026
Catching Up with Erin Venker
I first did a Q&A with Minnesota-based OCD therapist Erin Venker in 2017, the year she started taking clients. Then recently, she got in touch and asked if we could revisit some of her answers because her thinking has evolved over the years. I loved that she wanted to come back and share what she’s learned—it’s so important that therapists are willing to grow.
Erin cares deeply about the Twin Cities community as a whole and has held many events that bring people together, and she is committed to making access to care more equitable. Thank you, Erin!

What inspired you to create the Minnesota OCD Conference, and what do you hope attendees get out of it?
The Minnesota OCD Conference grew out of a gap I had seen for years, both as someone with OCD and as a clinician treating it. Minnesota has incredible providers, researchers, advocates, and lived experience voices, but too often they exist in silos. I wanted to create a space where all of those perspectives could be in the same room, learning from one another and building shared understanding.
The first Minnesota OCD Conference took place on October 11, 2025, and it was incredibly meaningful to see how well it was received. The response affirmed something I have long believed: people are hungry for accurate information, thoughtful dialogue, and real connection around OCD.
My hope for attendees was, and continues to be, that they leave feeling more connected, more informed, and less alone. Whether someone is an individual with OCD, a family member, or a professional, the conference is grounded in shared understanding. OCD thrives in isolation and misunderstanding, and community is one of the most powerful antidotes we have.
I also wanted the conference to raise the bar for how OCD is talked about, moving beyond stereotypes and toward nuanced, evidence-based, compassionate care. That same vision is guiding our next Minnesota OCD Conference on October 10, 2026, as we continue building something sustainable and community driven here in Minnesota.

You’ve hosted community events since founding OCDMN in 2017. What has stood out to you about bringing people together?
Some of the most meaningful moments for me have not been formal presentations. They have been the conversations that happen before and after events. People realizing, “Wait, you experience that too?” or “I didn’t know there was language for what I’ve been dealing with.”
Since 2017, we have hosted support groups, trainings, panels, and creative workshops. What stands out is how hungry people are for accurate information and safe connection. OCD can be deeply isolating, especially for people with taboo or misunderstood themes. Community events interrupt that isolation.
That is why this conference feels like a natural evolution rather than something entirely new.
Cultural sensitivity, equity, and access matter deeply to you. What would you like to say about that work?
I want to be honest here. As a white clinician, I do not get this perfect, and I never will. Cultural humility means staying open, self-critical, and accountable.
OCD does not exist in a vacuum. Culture, race, religion, immigration status, queerness, and systemic oppression all shape how symptoms show up, how people interpret them, and whether someone feels safe seeking care in the first place. Colonial frameworks in mental health have historically centered white, Western norms, and that has caused real harm.
At OCDMN, we aim to practice neurodivergent-, LGBTQ+-, and BIPOC-affirming care while also acknowledging our limitations. That includes listening to marginalized voices, continuing education, examining power dynamics, and building systems that reduce barriers to care rather than reinforcing them.
Equity is not a box you check. It is an ongoing practice.
You founded OCDMN in 2017. What has changed since then? Tell us about your team.
In 2017, OCDMN was essentially me, newly licensed, deeply motivated, and still learning what it truly takes to build sustainable, high-quality care. Today, we are a growing team of clinicians with specialized training in OCD, anxiety, neurodivergence, and related conditions.
What has changed most is clarity. We are unapologetically specialized. We invest heavily in training. We collaborate. We adapt as the field evolves. We have expanded beyond therapy alone to include assessments, professional education, community outreach, and now large-scale events like this conference.
The heart of the work has not changed, but the depth, structure, and reach absolutely have.
You mentioned revisiting earlier beliefs and treatment models. Can you talk about how your thinking has evolved?
I love this question because I believe therapists should change.
Earlier in my career, ERP was the clear centerpiece of my work, and it is still foundational. Over time, I have expanded how I conceptualize OCD. Inference-based CBT, or I-CBT, has profoundly shaped how I understand obsessional doubt, reasoning, and identity-based fear.
I have also become more precise about how and when different tools are used. DBT skills can be very helpful for emotional regulation and quality of life, but they are not OCD treatment on their own. Being clear about those distinctions matters.
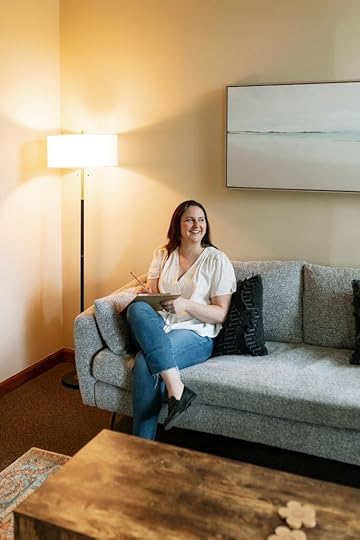
Growth does not mean abandoning what you knew. It means integrating new evidence and listening closely to clients.
You have OCD yourself. How long have you had it, and when did you realize that is what you were experiencing?
I first experienced OCD symptoms in elementary school, around fifth grade, though I was not formally diagnosed until seventh grade. Even then, I did not understand the full picture. I was too ashamed to talk about my intrusive thoughts, so I did not realize for many years that those thoughts were a core part of my OCD.
Like many people, I thought OCD was just rituals and visible behaviors. I did not yet have language for what was happening internally.
What were your symptoms like over time?
Early on, my OCD showed up as magical thinking, breathing rituals, lucky and unlucky colors, and the belief that my actions could control outcomes. That evolved into repetitive praying, confessing, and intense fear that I was responsible for harm coming to my family.
Later, my OCD became primarily mental, with rumination, replaying conversations, fear of offending others, reassurance seeking, and constant self monitoring. I had intrusive sexual and violent thoughts that felt unbearable. That period of my life is honestly blurry. I just remember how exhausting it was to exist inside my own mind.
What are your thoughts on the term “pure O”?
I am still nuanced about it.
Clinically, it is true that there are compulsions, often mental ones. Experientially, many people deeply identify with the term pure O, and that matters. I have worked with many individuals who did not seek treatment for years because they did not recognize their behaviors as compulsions.
For people with sexual, violent, or taboo intrusive thoughts, that lack of language can be devastating. They often fear they are dangerous or immoral rather than experiencing OCD.
If the term pure O helps someone recognize themselves and get help sooner, I see value in that.
Once you knew you had OCD, how did you treat it? When did relief begin?
I did not receive proper OCD treatment until about 14 years after my diagnosis. I spent years in well intentioned talk therapy that did not touch the core of OCD.
At 28, I began ERP with a specialist who understood the disorder deeply. Within a couple of months, I noticed real shifts. Not the absence of intrusive thoughts, but a change in how I related to them. That was life changing.
How do you use mindfulness now in OCD treatment?
Mindfulness helps create space between thoughts and meaning. For me, it is about observing rather than analyzing, judging, or solving.
Mindfulness works best when paired with evidence based OCD treatment. It is not about calming anxiety or making thoughts go away. It is about allowing uncertainty and disengaging from compulsive meaning making.
Used correctly, it supports ERP and I-CBT rather than replacing them.
How has your view on medication changed?
My view has matured. Medication can be essential, sometimes life saving, for people with OCD. What matters is thoughtful prescribing by providers who understand OCD and collaboration with therapy.
ERP and I-CBT remain core, but medication often makes engagement with treatment possible. I am increasingly vocal about that balance.
What is the hardest part of living with OCD?
The relentlessness. When OCD is loud, there is no mental rest. It is physically, emotionally, and cognitively exhausting.
I will also say this. People with OCD are often deeply thoughtful, creative, and values driven. Recovery is not about erasing sensitivity. It is about learning how to live alongside uncertainty.
If you could offer one piece of advice to others with OCD, what would it be?
Get specialized care. OCD requires specific treatment from clinicians who truly understand the disorder, and it should not be faced alone. Community matters.
OCD is painful and often misunderstood, but it is treatable. With the right support and evidence-based care, people can experience real relief, growth, and a fuller sense of themselves.
November 13, 2025
When OCD Is Misdiagnosed: Tracie Ibrahim
Ask Tracie Ibrahim—or “Taboo Tracie” on Instagram—to tell her OCD story, and you’ll likely walk away angry, sad, and in disbelief that she was treated so horribly as a kid and teen. And, you will be in awe of her. As she explains in more detail below, Tracie’s harm OCD was misdiagnosed, and she was in and out of psychiatric units for nearly a decade. When she finally received the right diagnosis as an adult, she made it her mission to treat kids and teens with OCD and make sure no one else experienced what she did. Tracie is hilarious, and she uses humor to take some of the sting out of taboo intrusive thoughts. Read on to get some of her advice, which I’ve tried myself!

I was lucky enough to hear you speak at an OCD event, and you said something that really stood out to me (though not so much I can remember it word for word, apparently): “If it’s horrific, it must be silly, so I’m going to laugh about it.” First, go ahead and tell us what you actually said. Then, can you tell us more about this strategy for addressing disturbing intrusive thoughts?
I think I said something like this: “If something feels terrifying, it’s likely ridiculous, so I’m just going to laugh about it.”
As someone who has been experiencing very graphic and detailed intrusive harm and sexual thoughts since I was 10 years old, I’ve learned that they are going to occur whether or I like it or not, and there is no way to escape them, but also there is no need to escape them. So much of what keeps OCD fueled up and loud is the many different types of mental and physical compulsions that people do while trying to escape or solve them. After decades of compulsing and living with out-of-control OCD symptoms, I learned that there is nothing to actually escape—there is no actual danger or concern that needs to be addressed at all. So I started thinking about it differently and started reacting differently when the intrusions would come up. I started using humor because I realized how absolutely ridiculous OCD is.

We know that trying to push thoughts away only makes them stronger, but it’s a natural first instinct. If someone isn’t ready to lean into their thoughts like you’re able to, what are some other approaches they can take?
I am a big fan of starting with a goal of identifying, reducing, and delaying compulsions. Maybe you aren’t ready to lean into the intrusive content just yet, but if you can truly commit yourself to focusing on doing some response prevention (reducing/delaying compulsions) then you will start to feel some amount of relief and then can work on doing more over time.
I love that you use humor to take OCD down a notch. There was a time when I thought I’d never find anything funny again, and I certainly didn’t think I’d be able to laugh at my darkest thoughts. Why do you think laughing at OCD is so powerful?
Using humor when it comes to OCD is what is technically called a “cognitive defusion” technique. This helps you observe your thoughts as separate events instead of 100 percent truths or facts, which reduces the power and grip they have on people with OCD. It breaks up the seriousness and helps you see it as ridiculous.
Your harm OCD was misdiagnosed when you were 10 years old, and you spent years in and out of varying levels of hospitalization. Can you walk us through some of that experience?
I recently posted on my Instagram a detailed timeline of events starting with my first misdiagnosis through three decades of absolutely nobody getting it right.
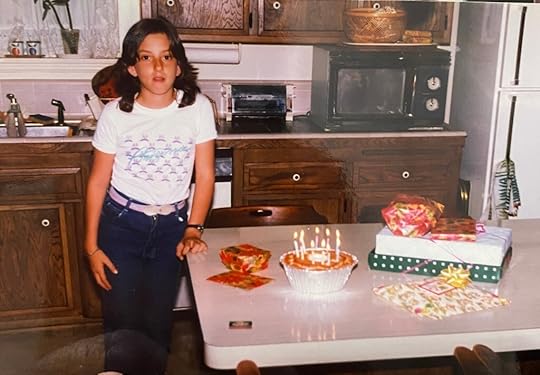
At age 10 I was going through difficult family issues and physical/emotional abuse by my stepfather. A series of events with the abuse led me to being taken in for a psychological evaluation. I was sad, crying, and scared. I never was suicidal or self-harming or anything like that. I was assessed as needing to be placed inpatient “to help ensure my safety and well-being.” Just like that, I was admitted to a children/teen psychiatric unit. I was diagnosed with depression. I was surrounded by teens who had attempted suicide, were self-harming, and had other disturbances. My undiagnosed OCD latched on to the question I was asked at my assessment, “Have you ever had thoughts, plans, or attempts to harm yourself or end your life?,” and then being surrounded by people who did in fact do those things only made it worse. I would meet with the psychiatrist and when asked if I was having any thoughts about harming myself or ending my life, I would answer “yes” because my intrusive thoughts and images were pounding in my brain even though I didn’t actually do anything at all and I never stated that I had a plan or intent to do any of those things. Nonetheless, I was placed on “suicide precautions” and that was the beginning of my decade of hell.
If I heard your story with no context, I’d assume it all happened in the 1950s. But it wasn’t that long ago! Do you think it would be less likely to happen today? What can mental health professionals and parents do to make sure no kid is involuntarily hospitalized like you were?
It is very common that OCD is misdiagnosed, even today, because the vast majority of therapists, psychiatrists, and other healthcare providers are not properly trained in how to assess or treat OCD and are not trained in all of the ways OCD can show up. I see it almost constantly. It’s one of the reasons I went into specializing in assessing and treating OCD in very young kids and teens, because I didn’t want this to keep happening. The best thing parents and caregivers can do is to ensure they are seeking professionals who are properly trained. It’s really difficult because a ton of professionals advertise themselves as “specializing” in OCD and OCD treatment, but they absolutely are out there doing harm, even if they think they know what they are doing. I would recommend only going to valid resources when looking for a care provider. Ensure they can educate you all about the various subtypes of OCD and that they were properly trained to utilize the gold-standard, evidence-based treatment for OCD, exposure and response prevention (ERP) therapy. This is not the same thing as exposure therapy, which actually makes things worse. Most practitioners were trained that regular CBT is how to treat OCD, but it treats OCD as if it is a logic disorder that can be cured with facts. That is simply untrue. OCD is not curable, but it is manageable, and you can live a full and beautiful life with ERP therapy.
After everything you went through as a kid and teen, I wouldn’t blame you if you wanted to get as far away from the mental health field as possible, but you decided you needed to help other kids as a therapist. Can you tell us about going to college after you’d been hospitalized for years?
I was angry, disappointed, damaged, and still improperly diagnosed and treated when I finally got out of the last mental health facility at almost 19 years old. I was still living with undiagnosed harm OCD (both suicidal and homicidal OCD) as well as other themes like contamination and just right OCD. I didn’t know how long I’d be alive, but I knew that I absolutely had to become a therapist who could offer better treatment to kids and teens who were suffering from mental illnesses like I was. So two weeks after I was discharged from the facility, I signed myself up for community college as a psychology major. I didn’t know exactly what was wrong with me or how to deal with it, but I at least wanted to help other kids and teens not have to feel as bad as I did and not have to suffer with incompetent care providers. I would help them feel better; I just needed to learn how to do it.

I finally got the right diagnosis at age 31 because I diagnosed myself with OCD and I found ERP treatment myself as well. That’s when everything changed and started getting better.
If you could give just one piece of advice to someone with OCD, what would it be?
Never ever give up. Don’t expect a treatment to “work for you” because it is you who has to do all of the hard work inside and outside of therapy sessions if you want to get better. There is no quick fix; it takes time and patience and perseverance to get better. OCD recovery is a lifestyle, not a destination.
October 30, 2025
Spreading Awareness Through Film: Tyler Falcoa and Mitch Francis
If you have obsessive-compulsive disorder (OCD), you probably don’t always love how it’s portrayed in TV shows, movies, books, commercials, jokes, daily life—anywhere, really. Thankfully, representation has gotten better and more accurate in recent years, due in large part to people with OCD creating meaningful projects that are touching and beautiful as well as educational. Today’s guests, Tyler Falcoa and Mitch Francis, have already made one short (and incredible) film about OCD, Do You Know How to Turn Off the Lights?, and are now working on a second one, Sorry I’m Late. Read on to learn more about both projects in their own words, including how you can support the production of Sorry I’m Late.
 Tyler Falcoa in Sorry I’m Late. Photo by Zack Francis.
Tyler Falcoa in Sorry I’m Late. Photo by Zack Francis.First, tell me a little about yourselves! Tyler, you have OCD, which you’re very open about as an IOCDF Advocate and host of the podcast Please Excuse My OCD. What made you decide to start spreading awareness? Was it scary?
Tyler: OCD has always been the wizard behind Oz in my life since I was a child. I first became “diagnosed” at the age of 10 after a traumatic football injury and house fire; however, I never really understood my OCD was what it was until I was 19 when my pediatrician pointed out that my horrific harm and suicidal intrusive thoughts were actually a symptom of my OCD. I got on medication at that time, but I still struggled with OCD throughout my 20s. It wasn’t until I learned about ERP, and unfortunately had done it by myself, where I started to notice changes in my life. I got my start being publicly open about my OCD in 2019. My brother Ryan, Mitch, and I had been very successful in building a YouTube music page, but we wanted to add something different to it. I had just gotten out of a six-month flare-up of existential OCD, and Mitch had asked me if I would be open to making a small documentary about it for the channel. We had no idea if people would care, but it turns out they very much cared. Fast-forward to 2024, I started the podcast Please Excuse My OCD, which gained quite a bit of support from others in the OCD community. I felt so welcomed by everyone who not only wanted to share their stories on the podcast but also help raise awareness within their own lives. It was the first time in my life where I truly felt understood. While there was some fear, I truly never felt like I was making the wrong decision by opening up about my OCD story publicly.
You’ve already made a short film about OCD, Do You Know How to Turn Off the Lights? What inspired it? How did your collaboration come about?
Tyler: I had written a spoken word in my Notes app on my phone one day for no reason at all but to simply see my thought process in front of me when I go through my bathroom routine when washing my hands. I figured if anything it could be a spoken word that I record and release on the podcast. I sent it to Mitch to see what he thought about it and he suggested we turn it into a full-on film.
 Tyler Falcoa in Please Excuse My OCD merch. Photo by Ryan Falcoa.
Tyler Falcoa in Please Excuse My OCD merch. Photo by Ryan Falcoa.Mitch: Tyler and I have worked together closely for years on different creative projects. When he sent me the poem he had written about OCD, I saw it in my head as I read it. I said we should make this into a film. He loved the idea. So I took the piece and adapted it into a screenplay and we made the film with just us two.
Now you’re working on a second film, a prequel to Do You Know How to Turn Off the Lights? You’ve said you plan to go all in on this one—one difference is that it will be longer than the first one, which was about five minutes long. What else can viewers expect this time around?
Mitch: With Sorry I’m Late, we’re expanding the world of the first film, both visually and emotionally. Do You Know How to Turn Off the Lights? took place entirely in one room, showing a single, isolated OCD spiral. This time, we’re stepping outside that space and following Tyler through an entire evening, seeing how those thoughts and rituals follow him into the real world.
The film will feel bigger, more cinematic, but it’s still intimate. We’ll explore more subtypes of OCD, like harm OCD, checking OCD, and pure O, to show how these thoughts don’t stop. They move with you, they warp how you experience the world, and they can turn something as simple as going to dinner into a mental battle.
We are expecting this film to be closer to 15 minutes long or so. Viewers can expect a film that goes deeper, not just into the condition, but into the humanity of living with it. It’s unsettling, honest, and deeply personal.
Tyler: I wrote Do You Know How To Turn Off The Lights? last year, expecting it to be a spoken word. Mitch had this idea to turn it into a film, which was absolutely the right move. I think with those details that Mitch shared, the differences will not only bring viewers closer to what OCD can feel like, but also expand upon what got my character to where he ended up in the first film. It all connects, which is something we’re excited about. Mitch wrote the screenplay for Sorry I’m Late and I will continue my role from the first one.
What do you hope they’ll walk away with?
Mitch: Our hope is the same. That people with OCD feel seen and understood. We want them to take these films to their loved ones and say, “This is what it’s like in my head.” Also, for people without OCD to see what it’s really like inside the mind of someone who lives with it every day, just for an evening.
 Mitch Francis. Photo by Ryan Falcoa.
Mitch Francis. Photo by Ryan Falcoa.Why is it important to make art about OCD?
Mitch: When we made Do You Know How to Turn Off the Lights?, people with OCD reached out saying, “This is the first time I’ve felt seen.” That meant everything.
These films are for anyone who lives with OCD and feels alone, and for everyone who wants to understand it better. If we can make even one person feel understood, or one person see OCD differently, then it’s worth everything.
Tyler: OCD is very much misunderstood, especially in the media. We feel it’s important to shed light on such a tough disorder because many of us already feel alone; we don’t deserve to feel misunderstood on top of that.
You’re raising funds to make the next film. Where can people donate? What can they do to help if they aren’t able to give money?
Mitch: People can support the film directly through our Indiegogo campaign. That’s where all donations go toward making Sorry I’m Late possible. Every contribution, no matter the size, helps us pay our small crew, rent the right equipment, and bring this story to life the way it deserves.
But support doesn’t have to be financial. Just sharing the campaign link, talking about the project, or telling someone about what we’re doing makes a huge difference. Even liking, commenting, or posting about it helps keep the conversation going. Because in the end, this isn’t just our film, it’s something we’re building with the community.
Every share, every voice, helps us tell this story to the people who need it most.
I ask all my guests this: If you could give just one piece of advice to someone with OCD, what would it be?
Mitch: You are not your thoughts. OCD will tell you otherwise, but you are so much more than what your mind throws at you. Thoughts are just thoughts, no matter how loud or convincing they feel.
Tyler: There can be a lot of shame associated with OCD. We often carry the world on our shoulders and feel responsible for anything “bad” that might happen. The truth is, leaning into the uncertainty, making choices, and moving even with the fear is where recovery often is found. It’s okay to be scared and do it anyway.
June 3, 2025
Remapping Recovery: A Study from Made of Millions
Earlier this year, Made of Millions—a nonprofit dedicated to helping the millions of people around the world who have a mental illness—published “Remapping Recovery: How Gen Z’s Quest for Better Care Is Pioneering New Paths Forward in Mental Health.”
Why this study, and why now? Aaron Harvey, co-founder of Made of Millions, said, “When we started in 2016, we used data that had been available for decades. So this research was an opportunity for us to better understand what the journey looks like for today’s youth, and specifically, how the internet’s democratization of mental health education and advocacy has shortened timelines and improved outcomes.”
As a person with a mental illness myself (but I’m part of Gen X, a generation that somehow sounds much closer to Gen Z than it is), I wanted to know more, especially the findings about my own diagnosis, obsessive-compulsive disorder (OCD), so I downloaded a copy. Some of the findings surprised me. Some of them gave me hope. And some of them confirmed that we still have work to do to make mental health care more accessible and inclusive.
When some of the gaps in access to mental health care are due to systemic inequality, it’s easy to feel overwhelmed, to feel a little hopeless and a little helpless. In the absence of sweeping systemic changes, what can we do to mitigate some inequities as we continue to fight? To be clear, I don’t believe the burden should be on the individual to fix a system, but I know I feel better when I can do something. To that end, I’ll include some ideas for getting help yourself or helping others.
What did Remapping Recovery find?But first, let’s go over some of the findings. These two stood out to me:
Gen Zs take nearly two times longer to research mental health conditions compared to their parents, but are also half as likely to report being misdiagnosed.
and
. . . in more than 90 percent of self-diagnoses, . . . Gen Zs are coupling their self-diagnosis with a professional one, or plan to.
They stood out to Lauren O’Shaughnessy of Made of Millions, too. She said, “These findings were surprising because there’s a popular narrative right now that social media is encouraging young people to abandon traditional healthcare altogether and attach themselves to the first mental health condition they stumble upon. This perspective undermines Gen Z’s intelligence and ability to self-educate.”
O’Shaughnessy said that it’s not a lack of wanting professional mental health care that keeps Gen Z from taking advantage of it. Rather, it’s the barriers to access: “financial constraints, long waitlists, and practitioner shortages,” she said.
What can be done?Gen Z are resourceful and will find information and support outside traditional systems. In an ideal world, this would only be a stopgap solution and would be supplementary, not a whole mental health care plan, but it’s important to know about the alternatives.
Esther Fernandez of Made of Millions said, “While it can be difficult to find someone who takes your insurance, there are definitely ways to tap into your community to see what is available to you. Using directories online is a good start. A local advocacy group might be hosting low-cost webinars, conferences, or support groups. A university might offer sliding-scale sessions with graduate students. Researchers might offer free medication or therapy sessions in exchange for research participation.”
What did Remapping Recovery find?“On average, it took respondents about 2.5 years between symptom onset and diagnosis.”
In the OCD community, we’ve been saying for as long as I can remember (actual decades) that the time period between onset of symptoms and diagnosis is 13 to 17 years. But this study’s respondents included kids under 18, a group that’s been omitted from other studies, and that time period is much, much shorter. (Keep in mind that Remapping Recovery isn’t a follow-up to those studies.)
Harvey credits this change at least in part to OCD advocates “who have spent the last decade making topics like intrusive thoughts part of our youth’s everyday vernacular.” Young people are finding community and non-stigmatizing information about mental illness online—and of course, they’re finding misinformation there as well.
A couple of years ago, I stumbled across a TikTok about taboo intrusive thoughts that was so stigmatizing it still upsets me. When I commented to explain that sexual and violent intrusive thoughts are a common symptom of OCD, the replies were from angry (and probably scared) people who don’t understand what OCD is. All I could think was How will this affect someone who hasn’t even started their recovery journey?
Helpful, well-researched videos about OCD—and other diagnoses—are abundant on TikTok and other social media sites, but one wildly wrong one can have a devastating impact if viewers don’t know how to determine which sources are credible.
What can be done?Uma Chatterjee, a member of Gen Z—oh, and neuroscientist, so she knows a little something about research—said, “Learn how to vet your sources and build literacy and you don’t have to understand everything. You have to understand who to look for and how to cross-check that information to make sure it’s accurate and it’s coming from someone who doesn’t have a vested interest in you being sick or buying their product cause they have the secret sauce to fix something that no one else has.”
The National Association for Media Literacy Education (NAMLE) outlines several questions people should ask to help determine whether the media they’re consuming is accurate and unbiased. Some include:
Who made this?Who was and was not involved in the creation of this?When was this made?Why was this made?What does it want me to do?Who is the target audience?Who paid for this?Who makes money from this?While these questions can be applied to any form of media, Fernandez said it’s important to note that social media is different from traditional media. For one thing, anyone with an account can (for the most part) post what they want. Fernandez said, “Just because someone has a large following doesn’t mean their content is credible. The algorithm is also tailored to you, so you might get caught in an echo chamber of information and communities pushing certain agendas. If your feed is full of influencers going viral talking about the same topics, you might start to believe that everything they say holds truth.”
If something on social media seems too good to be true—or maybe too bad or too unbelievable—don’t stop with that first source. See if that same information is published elsewhere, and if that other place is a credible source.
What did Remapping Recovery find?Eighty-five percent of Gen Zs either agree or somewhat agree that there’s a lot of stigma surrounding mental health, a number that increases to 90 percent among Gen Z Black, Indigenous, and People of Color (BIPOC). In fact, BIPOC respondents were 33 percent more likely to say that facing social stigma was one of the most difficult parts of their journey.
Chatterjee, who is brown, said reducing stigma in the BIPOC community largely falls to two groups of people: (1) Members of marginalized communities who have a diagnosis themselves and (2) allies. Beliefs about mental illness can be so deeply rooted, it is difficult to change the minds of folks in older generations, and without their support, younger generations are less likely to learn about mental illness or access helpful resources.
“You would think that educating peers would be easier,” Chatterjee said, “and that’s often just not true because they also grew up in the same type of stigma and they don’t have the ability to fight the stigma they have internalized about it, which means they won’t get help. So it’s just really isolating.”
What can be done?When BIPOC are expected to shoulder the burden of reducing the stigma surrounding their own mental health diagnosis, it only adds to the inequities they face in other aspects of life.
While nothing can replace being accepted and understood by their own families and communities, “I think there’s more that people can do who are not part of these communities,” Chatterjee said, “like providing friendship and support and going out of your way to create spaces for validation. It’s nice to invite someone to a [mental health] conference, but you can also invite them over to your house and ask them how they’re doing and see if there’s anything they need, like a meal.”
Most of the “tips” in the “What can be done?” sections are far bigger actions than anyone with a mental illness should have to take on, and I want to reiterate that what is really needed is an overhaul to systems in the United States. But in the meantime, let’s try to chip away at it with community, support, and educational resources that don’t require an appointment, insurance, money, or a world where stigma and inequities aren’t real barriers to evidence-based care. Studies like Remapping Recovery matter because they shine a light on gaps that are hurting people with mental illness.
December 8, 2024
Understanding I-CBT: Mike Heady
Hello! It’s been a while. I’m back now because over the past couple of years I’ve been seeing and hearing more about a new-to-me type of therapy for obsessive-compulsive disorder (OCD), inferenced-based cognitive behavioral therapy (I-CBT). I’ll be frank: I didn’t get it. I can explain exposure and response prevention (ERP) in about a minute, and that includes an example of how it works. I can’t do that with I-CBT—I’ll start to try to explain it to people and I have to stop. That’s frustrating! That’s why I asked Mike Heady to answer a bunch of my questions, which he very graciously did—including my follow-up questions. This is a long one, but I hope you find it helpful.

I was diagnosed with OCD over eighteen years ago, and one of the first things I learned about it was that the “gold standard” treatment was exposure and response prevention (ERP). In the past couple of years I’ve started to hear more about I-CBT. Full transparency: I’ve read a few articles about it, listened to a presentation on it, and attended a panel with OCD therapists who implement it with their clients and I still don’t understand it. I know I’m not the only one who’s a little confused, especially after years of telling people ERP is the best way to treat OCD. I invited you here because you were recommended as someone who’s well versed in I-CBT, and I genuinely want to understand how it all works.
First, tell me about yourself! How long have you been an OCD therapist, and how did you decide to focus on OCD? How long have you been using I-CBT with your clients? Do you still use ERP?
I have been specializing in the treatment of OCD, anxiety disorders, and related conditions for 17 years. After I graduated with my masters, I applied for a year-long mentorship program with the Anxiety & Stress Disorders Institute of MD. Think of it as a post-doc. I had the pleasure of shadowing some incredible clinicians like Carl Robbins and Sally Winston. While I was in the mentorship, I was also an adjunct professor of psychology at McDaniel College where I taught part-time for 10 years. Today, I am one of the owners and directors of the Institute. My decision to focus on these disorders is a mixture of being a fellow anxious person and being committed to understanding the unique puzzle these disorders present. I love to learn how and why things work which, in turn, informs how you approach them.
I began learning I-CBT in 2018 when Carl Robbins, our director of training, brought it to my attention. He had a few email correspondences with the late Kieron O’Connor, who is the co-developer of the approach. Carl was captivated and his curiosity and excitement rubbed off on me. In March of 2020 when the COVID-19 pandemic caused a shutdown, I was able to really dive into the I-CBT manual and start implementing it. So, it’s fair to say I’ve been using I-CBT for just over four years.
In my clinical practice, I continue to use ERP from an ACT-informed perspective when needed. It’s just now I am able to offer clients options that I could not before.
Pretend you’re in line for coffee at the OCD conference and you only have a minute—literally 60 seconds—to explain I-CBT to the person behind you. You have to grab your coffee and go, Mike! What do you say?
I would probably offer you an analogy. Imagine you are attending the best magic show to ever be. This magician is doing the impossible because you are watching an object disappear right before your eyes. You know things don’t just disappear but that is what you experience. You cannot explain it and for a moment you question your senses and reality itself. I-CBT shows you the magician’s secrets to how the illusion was pulled off. The sleight of hand. The misdirection. The showmanship of it all. Now imagine after you learn these secrets, you attend the show again. Do you remain tricked? I-CBT isn’t about tolerating fear or focusing on effortfully removing compulsions. Not that there is anything wrong with those approaches. I-CBT is about showing you how obsessions formed and tricked you into thinking you were in danger or that you were the danger when you clearly are not. If one knows and trusts the obsession to be irrelevant, what is left of OCD?
Now pretend you’re relaxing in the lobby. You have all the time in the world, and someone approaches you and says, “I understand ERP, but I want to learn more about I-CBT. Tell me everything. How does it work? When did it come about? What is research saying about its efficacy?”
I-CBT began when Kieron O’Connor observed that obsessions commonly took the form of a conclusion about a circumstance in the here and now rather than an intrusive thought that got stuck because it was scary. This seemingly innocuous observation has serious implications for how OCD is understood and how it’s treated. Basically, I-CBT would suggest that obsessions are faulty conclusions to doubt something about the here and now that ought not be doubted. They are obsessional doubts as opposed to normal doubts. Obsessional doubts are unique to those with OCD and related conditions (body dysmorphic disorder, eating disorders, and hoarding). There are several reasoning devices that are collectively referred to as inferential confusion, and I-CBT aims to deconstruct these processes through a series of modules, thus helping the client remove obsessional doubting (aka inferential confusion) and re-orient trust back into how they reason (normal reasoning) in all other areas of their life.
If we take the stereotypical case of hit-and-run OCD, a person driving a car to work runs over a pothole and within seconds is feverishly checking mirrors and trying to figure out if they hit someone, and eventually they turn around to check the sides of the road just in case. What happened in those moments, according to this approach, were not intrusive thoughts of maybe hitting a person that were taken as credible because they were scary and sticky. Rather, it was a reasoning process that was initiated once the pothole was hit, which is true of literally everyone who hit that pothole that day, with a significant exception. Most everyone else reasoned that the pothole may have damaged their tire or rim, which led them to keep an eye out for a wobbly car or a low tire pressure signal. But the person with OCD had a very different reasoning process with that pothole. They concluded that it could have somehow been a person rather than a pothole. And this conclusion felt absorbing and credible and urgent. How it was that they concluded what they did and why that conclusion was so credible and absorbing is where I-CBT focuses treatment. In this way I-CBT is said to work upstream from standard treatment models. It does not focus on fear and compulsions, but rather preceding reasoning processes that set them in motion.
Here is a schematic to illustrate this process:

Summary of Data/Efficacy:
It was in 1995 that the first theoretical paper with this observation about how obsessions come about was published. Four years later the first empirical investigation into this kind of doubting process was published by Paul Emmelkamp and Fred Aardema. Eventually, these distinct reasoning processes were collectively operationalized into a process referred to as inferential confusion. In the 25 years since, dozens of peer-reviewed studies on inferential confusion have validated it as a significant predictor of OCD independent from negative mood states and the obsessive beliefs categories noted by the obsessive-compulsive cognitions working group (OCCWG), which were inflated responsibility, perfectionism, intolerance for uncertainty, importance of thoughts, the need to control thoughts, and the overestimation of threat.
There is mounting data showing inferential confusion and feared self predicts OCD symptoms before any of the belief domains arise. This mediator analysis, which was a large replication study of 350 people diagnosed with OCD, demonstrated that inferential confusion and feared possible self sequentially mediated OCD symptoms completely independent of all obsessive belief domains and negative mood states and by itself explained 42 percent of the total variance of OCD. And, since I-CBT accepts that belief domains are relevant in OCD, despite them being downstream processes of inferential confusion and feared self processes, when we add relevant belief domains, total explained variance is about 58 percent, which is very significant. Data is mounting that shows inferential confusion as a mechanism of change, meaning that the resolution of inferential confusion predicts the reduction in OCD symptoms. Approximately six peer-reviewed studies showed this. In fact, a soon-to-be-published moderator analysis of a multisite randomized controlled trial (RCT) that looked at I-CBT, ERP, and mindfulness showed that the only cognitive process to predict the OCD symptom reduction in all groups was inferential confusion. This was directly compared to intolerance for uncertainty/perfectionism, importance and control of thoughts, and responsibility/threat. Aside from data validating inferential confusion as a central cognitive factor in OCD there is also data supporting numerous meaningful distinctions between normal intrusive thoughts that we all get and those that are relevant to OCD. For a more detailed description of these differences see Audet et al. (2020).
Once inferential confusion was demonstrated as distinct from other cognitive factors suggested by other treatment models, a new treatment model was constructed with the explicit purpose of resolving inferential confusion. This treatment was originally called inference-based therapy (IBT) and is now called inference-based CBT (I-CBT). It is primarily a cognitive treatment in that no deliberate or prolonged contact with distress (i.e., exposure) is required nor is any deliberate response prevention. The treatment focuses on helping the client build awareness of how they reasoned themselves into the obsessional doubting (faulty conclusion) so that they can return to their normal reasoning that they trust in all non-obsessional areas of functioning.
The first randomized controlled trial by O’Connor et al. was published in 2005. It showed two important outcomes: First, ERP and I-CBT were both equally effective at reducing OCD symptoms (neither was superior) and the second was that I-CBT appeared to be superior to ERP in helping a subgroup of those OCD sufferers with overvalued ideation. This RCT was small and needed replication in a larger sample. In 2015, an independent lab in the Netherlands conducted the second RCT with a larger sample and replicated the findings of the first RCT. In 2016, a large open trial with a waitlist control group demonstrated I-CBT to be effective across all OCD symptoms dimensions and showed that reduction in inferential confusion predicted the reduction in OCD symptoms. In 2022, the third RCT replicated yet again that I-CBT shows similar effectiveness as ERP at reducing OCD symptoms (neither treatment was superior). Most recently, the group in the Netherlands published a very large (about 100 participants per group) RCT with a non-inferiority design to see if I-CBT was equivalent to ERP as well as whether I-CBT was a more acceptable treatment option. Results on equivalence were inconclusive and both treatments were again shown to be similarly effective at reducing OCD symptoms. However, regarding treatment acceptability, I-CBT was found significantly superior to ERP. Treatment acceptability was measured with the Treatment Acceptability/Adherence Scale. Overall, participants in the I-CBT group found it less exhausting, less distressing to engage with, and less intrusive to their lives compared to the CBT/ERP group. I-CBT was also rated as less likely to drop out of compared to the CBT/ERP group (Wolf et al., 2024). A soon-to-be-published RCT, this one also with a non-inferiority design, will clarify the equivalence of I-CBT to ERP. This means to date there are six controlled trials testing I-CBT’s effectiveness and all agree that I-CBT is effective and not inferior or superior to ERP, albeit, more tolerable.
The body of research supporting I-CBT is substantial and growing. Approximately 100 peer-reviewed studies from independent labs across the world are demonstrating inferential confusion to be a central cognitive factor in OCD as well as I-CBT as a safe and effective treatment for adults with OCD. A growing body of evidence is demonstrating the relevance of feared possible self to OCD symptoms as well as its mediating role between inferential confusion and OCD symptoms. All this to say that the data points toward I-CBT’s assertion that inferential confusion and feared possible self precede other known cognitive factors in the development of OCD.
Can you break down how I-CBT would address the hit-and-run example above? What would you say to the client? What exercises would they work through? How would you know it’s “working”?
The how, in detail, is complex. [Kieron O’Connor wrote a breakdown of a case study that will help explain it, in addition to the description provided below.] I will briefly elaborate on a few modules here but not all.
In the case of hit-and-run OCD, I-CBT would focus on the initial doubt (what if that was a person?) and begin the 12 modules. The first 4 modules are considered psychoeducational. There is not challenging; rather, there is information gathering and organizing. Let’s look module by module how hit-and-run OCD would be addressed:
Module 1: The OCD sequence and identifying the initial doubt. The goal is to help the client be able to organize numerous OCD stories into the sequence and identify the initial doubts. In addition to this, the client also notes that the problem began with the doubting, not with the trigger or with any other part of the sequence. If the doubting were resolved, what would be left?
Hit-and-run OCD sequence:
Trigger: Drove over pothole
Doubt: What if that was a person?
Consequence of the doubt: A person could be hurt or dead.
Emotion: Guilt, fear
Compulsion: Check mirrors, check memory, turn car around to look for body, scan newspaper for report of a hit-and-run, etc.
Module 2: The doubt has its reasons. From the vantage point of the OCD, what about this doubt makes it convincing? Why attend to it rather than discard it? Here the goal is to hear out the client’s reasoning. It’s a validation of what goes on in their mind. We categorize the reasons into Possibility, Hearsay, Personal Experience, Out of Context Facts, and General Rules. The client would apply this to other OCD examples not necessarily their own but to get competent with the reasons.
If I hit a person I would feel a bump and I did feel a bump (out-of-context fact).
Hit-and-runs do occur so its not impossible that I did it (possibility).
Good drivers keep their eyes on the road and I might not have been perfectly attending to the road (general rules).
I heard that distracted drivers are more likely to hit pedestrians (hearsay).
When I was a teen learning to drive I hit a mailbox because I wasn’t paying attention, so that means I am prone to being a distracted driver (personal experience).
Module 3: The obsessional story. Obsessional doubts are not removed from our normal construction of reality, which means they are embedded in a story. The story is powerful in its ability to make things feel real and credible, so we demonstrate the power of the story and how a story’s ingredients absorb you into its reality. In this module the client is made aware of how stories generate a credible account of events even if imagined. Lastly, the client produces a counter-story for their OCD that starts from the same trigger but ends with a different conclusion (it was a pothole or debris that I ran over…). This is not to dispute or refute the obsessional story but rather to bring awareness to the availability of numerous stories that could be constructed with the same triggering event and that their specific obsessional story was just one of many possible stories.
Module 4: Feared possible self. Why this theme of OCD and not another? Here the client explores what underlying vulnerability set them up to reason with the pothole in this way rather than a completely different non-harm OCD situation. We help the client reveal that they have a story about the self that creates a hypervigilance for here-and-now circumstances that are relevant to being a negligent, irresponsible, careless or evil, bad, immoral, polluted . . . kind of person.
Modules 5–8 are intervention modules.
Module 5: OCD doubt is 100 percent imaginary. Here we help the client explore normal versus obsessional doubting. How they are constructed differently. It is their construction that renders them imaginary or not. Through examples the client gets competent at this distinction and then applies their understanding to their own doubting. They will see it is constructed obsessionally (through inferential confusion) and therefore is imaginary or hypothetical and not reality in the here and now.
Module 6: OCD doubt is 100 percent irrelevant. If the doubt is obsessionally constructed and not normally constructed then it is not relevant to the here and now. We explore why possibility is not relevant to reality by itself. We explore how all of the reasons OCD uses do not make the doubt relevant to the here and now. We explore what information would need to exist to make the doubt relevant to the here and now.
Module 7: The OCD bubble. Here we explore the absorbing and dissociative nature that inferential confusion creates. It lures you into its bubble where you are removed from reality in the senses and common sense and instead attend to possibilities and imaginations as more credible and relevant than reality through the senses. It goes into how OCD feels real and credible and urgent by disconnecting you from the present moment. An experiential exercise highlights the crossover point where you were in reality and then were absorbed into the OCD bubble and floated away from reality into your imagination.
Module 8: Reality sensing. Now that you are aware of obsessional versus normal doubting and understand all the ways in which this imagined and irrelevant story has tricked you, you now practice getting in contact with your senses and common sense in previously obsessional circumstances. This means the driver with hit-and-run OCD uses their five senses and common sense to drive down avoided roads and act upon what the senses are saying. If they hit a bump, they are trusting their senses rather than doubting them and indulging imaginations. Some of the practice here would be to help them connect to how they know anything about their present moment. How do you know when the chicken is cooked? How do you know when your spouse is upset with you? How do you know when the car is moving versus still? By making explicit how we know anything about the present moment (through senses) it is then generalized to their previously obsessional areas. This practice helps the client realize they already use and trust their senses without effort in everyday circumstances. Now we just ask them to do that normal sense work in the circumstances where the OCD bubble had previously caused distrust.
Module 9–12: Consolidation/relapse prevention
Module 9: The alternative story. Client is now rooted in reality with their previously obsessional circumstances, and we help them generate a more reality-based story. This story is an elaboration on the module 3 counter-story, but we add in how and why the client knows, through five senses and common sense, that their drive down a bumpy road is just that, a bumpy road. This story is rehearsed in non-obsessional moments (so it does not act as a disputation or refutation or compulsive reassurance). Again, this is not to replace the OCD story but to create an alternative option to be available to the client. Which do we trust and know to be real and which comes from the imagination?
Module 10: Tricks and cheats of the OCD con artist
Module 11: The real self
Module 12: Relapse prevention
While the last three modules are important, they are more connected to resolving the inferential confusion about the self (aka feared possible self) and then troubleshooting problems.
Each module has in-session worksheets, homework, and quizzes to test learning objectives. This is used at the discretion of the clinician based on client need. In short, you know the model is working when the client begins to trust their senses and self in day-to-day moments instead of getting lost in obsessional narratives. A signal of this could be the removal of compulsions and avoidances on their own volition or because it just made sense to not do the compulsions. If one is regimented in their clinical style they could administer the Y-BOCS and Inferential Confusion Questionnaire pre-treatment, midway through treatment, and post-treatment. Scores should ultimately drop below 92 to be in subclinical range. I usually just let my client report back how they are doing.
In summary, I-CBT systematically helps the client reorient themselves to their senses and common sense in situations where OCD had coaxed them away. Through a series of cognitive processes and experiential exercises, the client learns that they have been tricked by a clever and immersive faulty reasoning process applied to selective situations that drew them further into the land of the hypothetical and imagination. In effect, I-CBT breaks the obsessional doubting spell by showing you how it was constructed, selectively applied, and in contrast to how you reasoned in all other areas of living.
Something I’ve been having trouble understanding is how to avoid a spiral into compulsions while engaging in I-CBT. If you told me certainty was possible, I’d want proof of that. If you mentioned reasoning I could easily start to question why I have the obsessions I do—that was a huge problem for me and something I still struggle with. How do you make sure your client doesn’t devolve into reassurance seeking while on their path to certainty?
From an I-CBT perspective, obsessional doubt is when the person has knowledge about a situation in the here and now and then doubts this knowledge. The how and why one doubted is what I-CBT addresses directly. It offers insight into why this obsession and not others and yes, certainty in one’s senses and self in the here and now is as available for those with OCD as those without OCD. The former doubt what they know. While it is true to note that no one has certainty about the future it is also a red herring. Obsessional doubting is occurring in the here and now, as are the compulsions, not the future. There is sensory and common sense data here and now and those with OCD are reasoning with that information and drawing conclusions in the now. In this way, I-CBT is not disputing or refuting one’s thoughts but rather discovering the process of how they arrived at conclusions about themselves and the world.
The chance of OCD trying to misuse treatment as a compulsion is present for all treatment approaches. So long as one is being guided by a knowledgeable therapist, I think the risk of I-CBT facilitating compulsions is no different than ERP.
And do I have it all wrong? Does I-CBT not say certainty is possible? If it doesn’t, why do you think I could have gotten the impression it does?
Yes, there is certainty; however, I-CBT does not say there is certainty about the future, nor does it say there is certainty in situations that lack sufficient information to draw reasonable conclusions of knowing. For instance, imagine you applied to five universities and have a favorite, but you have yet to hear anything back from the schools. The doubt—what if I didn’t get into my college of choice?—is an example of a situation where not enough information is available to know. Another example: Imagine your doctor orders a biopsy of a lump and it’s not back yet and you say, what if my biopsy results show cancer?
These are all example of situations where there isn’t enough information to know, so true uncertainty exists and must be tolerated. However, if someone says, “What if that pothole was a person?” or “What if I am a violent serial killer?” these situations have available sensory and common sense information (which we all have) that lead to knowing. Those with OCD doubt this knowing. Think of it this way: If you came home from work and saw smoke and flames rising from your house, would you dismiss that sensory and common sense data and instead conclude that I might just be seeing things and you can’t know anything for sure and maybe it’s on fire, maybe it’s not, guess I’ll have to tolerate not knowing? Of course not. You would call 911 and say your house was on fire. You have certainty your house is on fire. So yes, certainty exists in this way and those with OCD have similarly available here-and-now sensory data to know the obsession isn’t true, but they doubt that information. Again, I-CBT is interested in showing you the how and why you doubt this way and how to resolve it.
When I’ve talked to fellow OCD-havers about I-CBT, some of them have said they don’t think they could easily engage with their senses because testing their physical reactions to obsessions is a compulsion. Let’s say someone has pedophilia OCD and they feel arousal but their therapist has just told them to trust what their body is telling them in the moment. How would you ensure they don’t now believe they really are a pedophile because their body has sent them the message that they are?
There is no testing in I-CBT. I-CBT is more than an instruction to engage your senses so the treatment process cannot be taken out of context in this way. The non-concordant arousal you mention is an example of an out-of-context fact from an I-CBT perspective. It could be a fact that arousal occurred, but the context is what makes the information relevant to being a pedophile or not. I-CBT specifically addresses this kind of irrelevant association that OCD uses to confuse you. The same argument could be used for headaches and brain tumors. Sure, brain tumors are associated with headaches but there is a context that makes that association relevant or not. The devil is in these details.
Sorry, I didn’t mean that I-CBT asks clients to test themselves, but I understand how it came across that way. It’s a concern I’ve heard people voice, that since they have struggled with the compulsion to test their senses (did I like that? Did my heartbeat speed up when I thought of stabbing someone? Did I feel it move?) they’re wary of the idea that they would be asked to trust their senses.
What’s an example of context that would make it irrelevant? What if the context is that someone is reading an article about Jeffery Epstein and how he brought girls to his island so people could have sex with them, and then you kinda picture it and you feel a sensation?
If someone reads about or hears about or pictures sex, it is within normal to experience signs of arousal. If I experienced arousal from tight-fitting pants, I am not desiring my pants nor does it speak to my orientation. Stimulation of any kind causes a response. By itself, arousal does not inform desire or consent. Yet the doubting is trying to make it so by inventing a possible context that does not exist, namely desire. (See the comment from your previous question–did I like that?) This is an example of a doubt. We know when we like something. We know when we desire and consent to something. If we are asking if we liked it, we are doubting.
Are there any types of OCD that I-CBT couldn’t treat as well as ERP?
Current evidence would suggest I-CBT is effective for all symptom dimensions of OCD (Aardema et al., 2017). However, to take it one layer further, I would say I-CBT treats all inferential confusion (obsessional doubting). There may be circumstances where a client looks to have OCD but it is really trauma or GAD where inferential confusion is not as significant a factor.
What is your position on using both I-CBT and ERP?
They can be used together or sequentially; however, care needs to be taken as these are very different interventions for different mechanisms of change. ERP pursues extinction learning via habituation or inhibitory learning. I-CBT pursues the resolution of inferential confusion. One needs to know the distinctions between these two mechanisms, so treatment is coherent.
A few modifications to ERP would remove much of the potential tension. First, focusing on in vivo or interoceptive exposures rather than imaginal exposures is suggested. Imaginal exposures as they are utilized in the RCTs of ERP, pursue the evocation and sustainment of distress often with efforts to increase the reality value of the imaginal script in the pursuit of extinction learning. This specific implementation would go against the effort to resolve inferential confusion as it deliberately draws on the imagination to absorb you into hypothetical scenarios to generate distress. The more reality value the better from the ERP perspective. The second is requiring the client to tolerate uncertainty about situations that do not require such toleration. As noted previously, certain doubts require tolerating uncertainty because there is not enough information to conclude knowledge, as in GAD; however, OCD doubting does not operate this way. These interventions implemented in these ways can create confusion for the client.
Otherwise, these approaches are not in conflict despite seeing OCD differently. In fact, there is data soon to be published that shows inferential confusion predicted OCD symptoms reduction in three treatment groups, I-CBT, MBSR, and ERP. So, ERP can reduce inferential confusion too, but it’s not required.
I’ve noticed division among therapists—some believe only ERP works for OCD, some believe I-CBT is better than ERP, and some are willing to try both as long as it works for their clients. Why do you think this has been a hot-button issue?
It’s unfortunate but not unexpected. Ultimately, I think it is because the contributions of I-CBT are challenging to the status quo. It is disruptive. Deeply held ideas are slow to adapt. I think of it as pushback rather than division. Some have felt that I-CBT advocates have made claims that outpaced the evidence others are concerned about leading young therapists astray. Neither of these criticisms are about the actual approach. They are more about qualms with isolated comments from individuals. I think these criticisms are equally applicable to CBT/ERP advocates as they are to I-CBT advocates and in my opinion, it’s not about those issues fundamentally. There has been occasional hairsplitting about what constitutes evidence-based which appears an almost moving target at times but to clear up any obfuscation, I-CBT is evidence-based. It satisfies all the fundamental pillars of empirical support for psychotherapies. To be reviewed by the American Psychological Association for their designation of “Empirically Supported Treatments” I-CBT needs to complete a meta-analysis. This is largely a procedural step, and it will be completed soon. More data is always needed but as it is today, I-CBT is a reasonable choice. It is listed as an evidence-based treatment for OCD by Scotland’s NHS.
I do not want to overemphasize the pushback either. By and large, the OCD community of clinicians and sufferers have embraced I-CBT. The community of clinicians interested in and learning about I-CBT in the US began with a dozen or so in 2021 and is now about 4,000 in 2024.
Understanding I-CBT with Mike Heady
Hello! It’s been a while. I’m back now because over the past couple of years I’ve been seeing and hearing more about a new-to-me type of therapy for obsessive-compulsive disorder (OCD), inferenced-based cognitive behavioral therapy (I-CBT). I’ll be frank: I didn’t get it. I can explain exposure and response prevention (ERP) in about a minute, and that includes an example of how it works. I can’t do that with I-CBT—I’ll start to try to explain it to people and I have to stop. That’s frustrating! That’s why I asked Mike Heady to answer a bunch of my questions, which he very graciously did—including my follow-up questions. This is a long one, but I hope you find it helpful.

I was diagnosed with OCD over eighteen years ago, and one of the first things I learned about it was that the “gold standard” treatment was exposure and response prevention (ERP). In the past couple of years I’ve started to hear more about I-CBT. Full transparency: I’ve read a few articles about it, listened to a presentation on it, and attended a panel with OCD therapists who implement it with their clients and I still don’t understand it. I know I’m not the only one who’s a little confused, especially after years of telling people ERP is the best way to treat OCD. I invited you here because you were recommended as someone who’s well versed in I-CBT, and I genuinely want to understand how it all works.
First, tell me about yourself! How long have you been an OCD therapist, and how did you decide to focus on OCD? How long have you been using I-CBT with your clients? Do you still use ERP?
I have been specializing in the treatment of OCD, anxiety disorders, and related conditions for 17 years. After I graduated with my masters, I applied for a year-long mentorship program with the Anxiety & Stress Disorders Institute of MD. Think of it as a post-doc. I had the pleasure of shadowing some incredible clinicians like Carl Robbins and Sally Winston. While I was in the mentorship, I was also an adjunct professor of psychology at McDaniel College where I taught part-time for 10 years. Today, I am one of the owners and directors of the Institute. My decision to focus on these disorders is a mixture of being a fellow anxious person and being committed to understanding the unique puzzle these disorders present. I love to learn how and why things work which, in turn, informs how you approach them.
I began learning I-CBT in 2018 when Carl Robbins, our director of training, brought it to my attention. He had a few email correspondences with the late Kieron O’Connor, who is the co-developer of the approach. Carl was captivated and his curiosity and excitement rubbed off on me. In March of 2020 when the COVID-19 pandemic caused a shutdown, I was able to really dive into the I-CBT manual and start implementing it. So, it’s fair to say I’ve been using I-CBT for just over four years.
In my clinical practice, I continue to use ERP from an ACT-informed perspective when needed. It’s just now I am able to offer clients options that I could not before.
Pretend you’re in line for coffee at the OCD conference and you only have a minute—literally 60 seconds—to explain I-CBT to the person behind you. You have to grab your coffee and go, Mike! What do you say?
I would probably offer you an analogy. Imagine you are attending the best magic show to ever be. This magician is doing the impossible because you are watching an object disappear right before your eyes. You know things don’t just disappear but that is what you experience. You cannot explain it and for a moment you question your senses and reality itself. I-CBT shows you the magician’s secrets to how the illusion was pulled off. The sleight of hand. The misdirection. The showmanship of it all. Now imagine after you learn these secrets, you attend the show again. Do you remain tricked? I-CBT isn’t about tolerating fear or focusing on effortfully removing compulsions. Not that there is anything wrong with those approaches. I-CBT is about showing you how obsessions formed and tricked you into thinking you were in danger or that you were the danger when you clearly are not. If one knows and trusts the obsession to be irrelevant, what is left of OCD?
Now pretend you’re relaxing in the lobby. You have all the time in the world, and someone approaches you and says, “I understand ERP, but I want to learn more about I-CBT. Tell me everything. How does it work? When did it come about? What is research saying about its efficacy?”
I-CBT began when Kieron O’Connor observed that obsessions commonly took the form of a conclusion about a circumstance in the here and now rather than an intrusive thought that got stuck because it was scary. This seemingly innocuous observation has serious implications for how OCD is understood and how it’s treated. Basically, I-CBT would suggest that obsessions are faulty conclusions to doubt something about the here and now that ought not be doubted. They are obsessional doubts as opposed to normal doubts. Obsessional doubts are unique to those with OCD and related conditions (body dysmorphic disorder, eating disorders, and hoarding). There are several reasoning devices that are collectively referred to as inferential confusion, and I-CBT aims to deconstruct these processes through a series of modules, thus helping the client remove obsessional doubting (aka inferential confusion) and re-orient trust back into how they reason (normal reasoning) in all other areas of their life.
If we take the stereotypical case of hit-and-run OCD, a person driving a car to work runs over a pothole and within seconds is feverishly checking mirrors and trying to figure out if they hit someone, and eventually they turn around to check the sides of the road just in case. What happened in those moments, according to this approach, were not intrusive thoughts of maybe hitting a person that were taken as credible because they were scary and sticky. Rather, it was a reasoning process that was initiated once the pothole was hit, which is true of literally everyone who hit that pothole that day, with a significant exception. Most everyone else reasoned that the pothole may have damaged their tire or rim, which led them to keep an eye out for a wobbly car or a low tire pressure signal. But the person with OCD had a very different reasoning process with that pothole. They concluded that it could have somehow been a person rather than a pothole. And this conclusion felt absorbing and credible and urgent. How it was that they concluded what they did and why that conclusion was so credible and absorbing is where I-CBT focuses treatment. In this way I-CBT is said to work upstream from standard treatment models. It does not focus on fear and compulsions, but rather preceding reasoning processes that set them in motion.
Here is a schematic to illustrate this process:

Summary of Data/Efficacy:
It was in 1995 that the first theoretical paper with this observation about how obsessions come about was published. Four years later the first empirical investigation into this kind of doubting process was published by Paul Emmelkamp and Fred Aardema. Eventually, these distinct reasoning processes were collectively operationalized into a process referred to as inferential confusion. In the 25 years since, dozens of peer-reviewed studies on inferential confusion have validated it as a significant predictor of OCD independent from negative mood states and the obsessive beliefs categories noted by the obsessive-compulsive cognitions working group (OCCWG), which were inflated responsibility, perfectionism, intolerance for uncertainty, importance of thoughts, the need to control thoughts, and the overestimation of threat.
There is mounting data showing inferential confusion and feared self predicts OCD symptoms before any of the belief domains arise. This mediator analysis, which was a large replication study of 350 people diagnosed with OCD, demonstrated that inferential confusion and feared possible self sequentially mediated OCD symptoms completely independent of all obsessive belief domains and negative mood states and by itself explained 42 percent of the total variance of OCD. And, since I-CBT accepts that belief domains are relevant in OCD, despite them being downstream processes of inferential confusion and feared self processes, when we add relevant belief domains, total explained variance is about 58 percent, which is very significant. Data is mounting that shows inferential confusion as a mechanism of change, meaning that the resolution of inferential confusion predicts the reduction in OCD symptoms. Approximately six peer-reviewed studies showed this. In fact, a soon-to-be-published moderator analysis of a multisite randomized controlled trial (RCT) that looked at I-CBT, ERP, and mindfulness showed that the only cognitive process to predict the OCD symptom reduction in all groups was inferential confusion. This was directly compared to intolerance for uncertainty/perfectionism, importance and control of thoughts, and responsibility/threat. Aside from data validating inferential confusion as a central cognitive factor in OCD there is also data supporting numerous meaningful distinctions between normal intrusive thoughts that we all get and those that are relevant to OCD. For a more detailed description of these differences see Audet et al. (2020).
Once inferential confusion was demonstrated as distinct from other cognitive factors suggested by other treatment models, a new treatment model was constructed with the explicit purpose of resolving inferential confusion. This treatment was originally called inference-based therapy (IBT) and is now called inference-based CBT (I-CBT). It is primarily a cognitive treatment in that no deliberate or prolonged contact with distress (i.e., exposure) is required nor is any deliberate response prevention. The treatment focuses on helping the client build awareness of how they reasoned themselves into the obsessional doubting (faulty conclusion) so that they can return to their normal reasoning that they trust in all non-obsessional areas of functioning.
The first randomized controlled trial by O’Connor et al. was published in 2005. It showed two important outcomes: First, ERP and I-CBT were both equally effective at reducing OCD symptoms (neither was superior) and the second was that I-CBT appeared to be superior to ERP in helping a subgroup of those OCD sufferers with overvalued ideation. This RCT was small and needed replication in a larger sample. In 2015, an independent lab in the Netherlands conducted the second RCT with a larger sample and replicated the findings of the first RCT. In 2016, a large open trial with a waitlist control group demonstrated I-CBT to be effective across all OCD symptoms dimensions and showed that reduction in inferential confusion predicted the reduction in OCD symptoms. In 2022, the third RCT replicated yet again that I-CBT shows similar effectiveness as ERP at reducing OCD symptoms (neither treatment was superior). Most recently, the group in the Netherlands published a very large (about 100 participants per group) RCT with a non-inferiority design to see if I-CBT was equivalent to ERP as well as whether I-CBT was a more acceptable treatment option. Results on equivalence were inconclusive and both treatments were again shown to be similarly effective at reducing OCD symptoms. However, regarding treatment acceptability, I-CBT was found significantly superior to ERP. Treatment acceptability was measured with the Treatment Acceptability/Adherence Scale. Overall, participants in the I-CBT group found it less exhausting, less distressing to engage with, and less intrusive to their lives compared to the CBT/ERP group. I-CBT was also rated as less likely to drop out of compared to the CBT/ERP group (Wolf et al., 2024). A soon-to-be-published RCT, this one also with a non-inferiority design, will clarify the equivalence of I-CBT to ERP. This means to date there are six controlled trials testing I-CBT’s effectiveness and all agree that I-CBT is effective and not inferior or superior to ERP, albeit, more tolerable.
The body of research supporting I-CBT is substantial and growing. Approximately 100 peer-reviewed studies from independent labs across the world are demonstrating inferential confusion to be a central cognitive factor in OCD as well as I-CBT as a safe and effective treatment for adults with OCD. A growing body of evidence is demonstrating the relevance of feared possible self to OCD symptoms as well as its mediating role between inferential confusion and OCD symptoms. All this to say that the data points toward I-CBT’s assertion that inferential confusion and feared possible self precede other known cognitive factors in the development of OCD.
Can you break down how I-CBT would address the hit-and-run example above? What would you say to the client? What exercises would they work through? How would you know it’s “working”?
The how, in detail, is complex. [Kieron O’Connor wrote a breakdown of a case study that will help explain it, in addition to the description provided below.] I will briefly elaborate on a few modules here but not all.
In the case of hit-and-run OCD, I-CBT would focus on the initial doubt (what if that was a person?) and begin the 12 modules. The first 4 modules are considered psychoeducational. There is not challenging; rather, there is information gathering and organizing. Let’s look module by module how hit-and-run OCD would be addressed:
Module 1: The OCD sequence and identifying the initial doubt. The goal is to help the client be able to organize numerous OCD stories into the sequence and identify the initial doubts. In addition to this, the client also notes that the problem began with the doubting, not with the trigger or with any other part of the sequence. If the doubting were resolved, what would be left?
Hit-and-run OCD sequence:
Trigger: Drove over pothole
Doubt: What if that was a person?
Consequence of the doubt: A person could be hurt or dead.
Emotion: Guilt, fear
Compulsion: Check mirrors, check memory, turn car around to look for body, scan newspaper for report of a hit-and-run, etc.
Module 2: The doubt has its reasons. From the vantage point of the OCD, what about this doubt makes it convincing? Why attend to it rather than discard it? Here the goal is to hear out the client’s reasoning. It’s a validation of what goes on in their mind. We categorize the reasons into Possibility, Hearsay, Personal Experience, Out of Context Facts, and General Rules. The client would apply this to other OCD examples not necessarily their own but to get competent with the reasons.
If I hit a person I would feel a bump and I did feel a bump (out-of-context fact).
Hit-and-runs do occur so its not impossible that I did it (possibility).
Good drivers keep their eyes on the road and I might not have been perfectly attending to the road (general rules).
I heard that distracted drivers are more likely to hit pedestrians (hearsay).
When I was a teen learning to drive I hit a mailbox because I wasn’t paying attention, so that means I am prone to being a distracted driver (personal experience).
Module 3: The obsessional story. Obsessional doubts are not removed from our normal construction of reality, which means they are embedded in a story. The story is powerful in its ability to make things feel real and credible, so we demonstrate the power of the story and how a story’s ingredients absorb you into its reality. In this module the client is made aware of how stories generate a credible account of events even if imagined. Lastly, the client produces a counter-story for their OCD that starts from the same trigger but ends with a different conclusion (it was a pothole or debris that I ran over…). This is not to dispute or refute the obsessional story but rather to bring awareness to the availability of numerous stories that could be constructed with the same triggering event and that their specific obsessional story was just one of many possible stories.
Module 4: Feared possible self. Why this theme of OCD and not another? Here the client explores what underlying vulnerability set them up to reason with the pothole in this way rather than a completely different non-harm OCD situation. We help the client reveal that they have a story about the self that creates a hypervigilance for here-and-now circumstances that are relevant to being a negligent, irresponsible, careless or evil, bad, immoral, polluted . . . kind of person.
Modules 5–8 are intervention modules.
Module 5: OCD doubt is 100 percent imaginary. Here we help the client explore normal versus obsessional doubting. How they are constructed differently. It is their construction that renders them imaginary or not. Through examples the client gets competent at this distinction and then applies their understanding to their own doubting. They will see it is constructed obsessionally (through inferential confusion) and therefore is imaginary or hypothetical and not reality in the here and now.
Module 6: OCD doubt is 100 percent irrelevant. If the doubt is obsessionally constructed and not normally constructed then it is not relevant to the here and now. We explore why possibility is not relevant to reality by itself. We explore how all of the reasons OCD uses do not make the doubt relevant to the here and now. We explore what information would need to exist to make the doubt relevant to the here and now.
Module 7: The OCD bubble. Here we explore the absorbing and dissociative nature that inferential confusion creates. It lures you into its bubble where you are removed from reality in the senses and common sense and instead attend to possibilities and imaginations as more credible and relevant than reality through the senses. It goes into how OCD feels real and credible and urgent by disconnecting you from the present moment. An experiential exercise highlights the crossover point where you were in reality and then were absorbed into the OCD bubble and floated away from reality into your imagination.
Module 8: Reality sensing. Now that you are aware of obsessional versus normal doubting and understand all the ways in which this imagined and irrelevant story has tricked you, you now practice getting in contact with your senses and common sense in previously obsessional circumstances. This means the driver with hit-and-run OCD uses their five senses and common sense to drive down avoided roads and act upon what the senses are saying. If they hit a bump, they are trusting their senses rather than doubting them and indulging imaginations. Some of the practice here would be to help them connect to how they know anything about their present moment. How do you know when the chicken is cooked? How do you know when your spouse is upset with you? How do you know when the car is moving versus still? By making explicit how we know anything about the present moment (through senses) it is then generalized to their previously obsessional areas. This practice helps the client realize they already use and trust their senses without effort in everyday circumstances. Now we just ask them to do that normal sense work in the circumstances where the OCD bubble had previously caused distrust.
Module 9–12: Consolidation/relapse prevention
Module 9: The alternative story. Client is now rooted in reality with their previously obsessional circumstances, and we help them generate a more reality-based story. This story is an elaboration on the module 3 counter-story, but we add in how and why the client knows, through five senses and common sense, that their drive down a bumpy road is just that, a bumpy road. This story is rehearsed in non-obsessional moments (so it does not act as a disputation or refutation or compulsive reassurance). Again, this is not to replace the OCD story but to create an alternative option to be available to the client. Which do we trust and know to be real and which comes from the imagination?
Module 10: Tricks and cheats of the OCD con artist
Module 11: The real self
Module 12: Relapse prevention
While the last three modules are important, they are more connected to resolving the inferential confusion about the self (aka feared possible self) and then troubleshooting problems.
Each module has in-session worksheets, homework, and quizzes to test learning objectives. This is used at the discretion of the clinician based on client need. In short, you know the model is working when the client begins to trust their senses and self in day-to-day moments instead of getting lost in obsessional narratives. A signal of this could be the removal of compulsions and avoidances on their own volition or because it just made sense to not do the compulsions. If one is regimented in their clinical style they could administer the Y-BOCS and Inferential Confusion Questionnaire pre-treatment, midway through treatment, and post-treatment. Scores should ultimately drop below 92 to be in subclinical range. I usually just let my client report back how they are doing.
In summary, I-CBT systematically helps the client reorient themselves to their senses and common sense in situations where OCD had coaxed them away. Through a series of cognitive processes and experiential exercises, the client learns that they have been tricked by a clever and immersive faulty reasoning process applied to selective situations that drew them further into the land of the hypothetical and imagination. In effect, I-CBT breaks the obsessional doubting spell by showing you how it was constructed, selectively applied, and in contrast to how you reasoned in all other areas of living.
Something I’ve been having trouble understanding is how to avoid a spiral into compulsions while engaging in I-CBT. If you told me certainty was possible, I’d want proof of that. If you mentioned reasoning I could easily start to question why I have the obsessions I do—that was a huge problem for me and something I still struggle with. How do you make sure your client doesn’t devolve into reassurance seeking while on their path to certainty?
From an I-CBT perspective, obsessional doubt is when the person has knowledge about a situation in the here and now and then doubts this knowledge. The how and why one doubted is what I-CBT addresses directly. It offers insight into why this obsession and not others and yes, certainty in one’s senses and self in the here and now is as available for those with OCD as those without OCD. The latter doubt what they know. While it is true to note that no one has certainty about the future it is also a red herring. Obsessional doubting is occurring in the here and now, as are the compulsions, not the future. There is sensory and common sense data here and now and those with OCD are reasoning with that information and drawing conclusions in the now. In this way, I-CBT is not disputing or refuting one’s thoughts but rather discovering the process of how they arrived at conclusions about themselves and the world.
The chance of OCD trying to misuse treatment as a compulsion is present for all treatment approaches. So long as one is being guided by a knowledgeable therapist, I think the risk of I-CBT facilitating compulsions is no different than ERP.
And do I have it all wrong? Does I-CBT not say certainty is possible? If it doesn’t, why do you think I could have gotten the impression it does?
Yes, there is certainty; however, I-CBT does not say there is certainty about the future, nor does it say there is certainty in situations that lack sufficient information to draw reasonable conclusions of knowing. For instance, imagine you applied to five universities and have a favorite, but you have yet to hear anything back from the schools. The doubt—what if I didn’t get into my college of choice?—is an example of a situation where not enough information is available to know. Another example: Imagine your doctor orders a biopsy of a lump and it’s not back yet and you say, what if my biopsy results show cancer?
These are all example of situations where there isn’t enough information to know, so true uncertainty exists and must be tolerated. However, if someone says, “What if that pothole was a person?” or “What if I am a violent serial killer?” these situations have available sensory and common sense information (which we all have) that lead to knowing. Those with OCD doubt this knowing. Think of it this way: If you came home from work and saw smoke and flames rising from your house, would you dismiss that sensory and common sense data and instead conclude that I might just be seeing things and you can’t know anything for sure and maybe it’s on fire, maybe it’s not, guess I’ll have to tolerate not knowing? Of course not. You would call 911 and say your house was on fire. You have certainty your house is on fire. So yes, certainty exists in this way and those with OCD have similarly available here-and-now sensory data to know the obsession isn’t true, but they doubt that information. Again, I-CBT is interested in showing you the how and why you doubt this way and how to resolve it.
When I’ve talked to fellow OCD-havers about I-CBT, some of them have said they don’t think they could easily engage with their senses because testing their physical reactions to obsessions is a compulsion. Let’s say someone has pedophilia OCD and they feel arousal but their therapist has just told them to trust what their body is telling them in the moment. How would you ensure they don’t now believe they really are a pedophile because their body has sent them the message that they are?
There is no testing in I-CBT. I-CBT is more than an instruction to engage your senses so the treatment process cannot be taken out of context in this way. The non-concordant arousal you mention is an example of an out-of-context fact from an I-CBT perspective. It could be a fact that arousal occurred, but the context is what makes the information relevant to being a pedophile or not. I-CBT specifically addresses this kind of irrelevant association that OCD uses to confuse you. The same argument could be used for headaches and brain tumors. Sure, brain tumors are associated with headaches but there is a context that makes that association relevant or not. The devil is in these details.
Sorry, I didn’t mean that I-CBT asks clients to test themselves, but I understand how it came across that way. It’s a concern I’ve heard people voice, that since they have struggled with the compulsion to test their senses (did I like that? Did my heartbeat speed up when I thought of stabbing someone? Did I feel it move?) they’re wary of the idea that they would be asked to trust their senses.
What’s an example of context that would make it irrelevant? What if the context is that someone is reading an article about Jeffery Epstein and how he brought girls to his island so people could have sex with them, and then you kinda picture it and you feel a sensation?
If someone reads about or hears about or pictures sex, it is within normal to experience signs of arousal. If I experienced arousal from tight-fitting pants, I am not desiring my pants nor does it speak to my orientation. Stimulation of any kind causes a response. By itself, arousal does not inform desire or consent. Yet the doubting is trying to make it so by inventing a possible context that does not exist, namely desire. (See the comment from your previous question–did I like that?) This is an example of a doubt. We know when we like something. We know when we desire and consent to something. If we are asking if we liked it, we are doubting.
Are there any types of OCD that I-CBT couldn’t treat as well as ERP?
Current evidence would suggest I-CBT is effective for all symptom dimensions of OCD (Aardema et al., 2017). However, to take it one layer further, I would say I-CBT treats all inferential confusion (obsessional doubting). There may be circumstances where a client looks to have OCD but it is really trauma or GAD where inferential confusion is not as significant a factor.
What is your position on using both I-CBT and ERP?
They can be used together or sequentially; however, care needs to be taken as these are very different interventions for different mechanisms of change. ERP pursues extinction learning via habituation or inhibitory learning. I-CBT pursues the resolution of inferential confusion. One needs to know the distinctions between these two mechanisms, so treatment is coherent.
A few modifications to ERP would remove much of the potential tension. First, focusing on in vivo or interoceptive exposures rather than imaginal exposures is suggested. Imaginal exposures as they are utilized in the RCTs of ERP, pursue the evocation and sustainment of distress often with efforts to increase the reality value of the imaginal script in the pursuit of extinction learning. This specific implementation would go against the effort to resolve inferential confusion as it deliberately draws on the imagination to absorb you into hypothetical scenarios to generate distress. The more reality value the better from the ERP perspective. The second is requiring the client to tolerate uncertainty about situations that do not require such toleration. As noted previously, certain doubts require tolerating uncertainty because there is not enough information to conclude knowledge, as in GAD; however, OCD doubting does not operate this way. These interventions implemented in these ways can create confusion for the client.
Otherwise, these approaches are not in conflict despite seeing OCD differently. In fact, there is data soon to be published that shows inferential confusion predicted OCD symptoms reduction in three treatment groups, I-CBT, MBSR, and ERP. So, ERP can reduce inferential confusion too, but it’s not required.
I’ve noticed division among therapists—some believe only ERP works for OCD, some believe I-CBT is better than ERP, and some are willing to try both as long as it works for their clients. Why do you think this has been a hot-button issue?
It’s unfortunate but not unexpected. Ultimately, I think it is because the contributions of I-CBT are challenging to the status quo. It is disruptive. Deeply held ideas are slow to adapt. I think of it as pushback rather than division. Some have felt that I-CBT advocates have made claims that outpaced the evidence others are concerned about leading young therapists astray. Neither of these criticisms are about the actual approach. They are more about qualms with isolated comments from individuals. I think these criticisms are equally applicable to CBT/ERP advocates as they are to I-CBT advocates and in my opinion, it’s not about those issues fundamentally. There has been occasional hairsplitting about what constitutes evidence-based which appears an almost moving target at times but to clear up any obfuscation, I-CBT is evidence-based. It satisfies all the fundamental pillars of empirical support for psychotherapies. To be reviewed by the American Psychological Association for their designation of “Empirically Supported Treatments” I-CBT needs to complete a meta-analysis. This is largely a procedural step, and it will be completed soon. More data is always needed but as it is today, I-CBT is a reasonable choice. It is listed as an evidence-based treatment for OCD by Scotland’s NHS.
I do not want to overemphasize the pushback either. By and large, the OCD community of clinicians and sufferers have embraced I-CBT. The community of clinicians interested in and learning about I-CBT in the US began with a dozen or so in 2021 and is now about 4,000 in 2024.
November 1, 2023
Finding Community: Michael Schramm
Please help me welcome Michael Schramm, one of the nicest and most positive people I know! He is truly a day brightener, and I’m so happy to host him today and learn more about his experience with OCD. If you live in the Wichita, Kansas, area be sure to see him—and other amazing advocates and therapists—speak at the OCD Gamechangers event this weekend.
You’re about to share your personal experience with OCD at an OCD Gamechangers event in Wichita, Kansas. Why did you decide to tell your story on stage?

I decided to tell my story on stage because I know how isolating having OCD can be, and if it helps someone in the audience feels less alone, it is absolutely worth it. When I was diagnosed at 16 this was a disorder I knew nothing about, and didn’t know anyone who had OCD that I could relate to and have that bond with. By telling my story I hopefully can be someone that the audience can have that feeling of you know what? I am not as alone in this as I thought I was, that there are other people that I can talk to and keep in touch with.
The other reason is to show myself how far I have come in my own OCD journey; I never thought for the longest time that I could do something like this. When I experienced my first Gamechangers event in 2020 I thought it was so incredible how all these people where sharing their stories, and I thought that would be great if I could do the same one day, and here I am getting ready to do the exact thing that in 2020 I dreamed of doing. To show myself that OCD doesn’t get to dictate everything I do.
Give us a little sneak peek of what you’ll be sharing: When were you diagnosed with OCD, and how long did you have symptoms before you realized that you might have OCD?
I was diagnosed with OCD at the age of 16 in 1998 at Menninger Clinic in Topeka, Kansas. I had been receiving therapy all throughout my childhood. My symptoms started at a very young age around 5 or 6. The first intrusive thought I remember was when I was coming home on the school bus a girl got sick on the bus. I was worried I couldn’t get back on the bus because if I did I would get sick on the bus. It got so bad my mom had to start riding the bus with me; when that didn’t work my mom had to start driving me to school for a while. The other memory I had when I was child was having visions of people in my head called The Spirit People that resembled what I thought looked like Jesus. They would tell me I would have to do things like tap a certain number of times, or walk between the couch and the chair or something bad would happen to my family. It wasn’t until I was a freshman in high school that my talk therapist suspected I had OCD. She referred me to an OCD specialist at Menninger Clinic and he diagnosed me as having OCD.
Once you knew you had OCD, did you tell friends and loved ones? If so, how did you go about it? Were you nervous to do it, relieved to get it out, happy to finally talk about it?
We told family members for sure, because I had such a difficult childhood with all that had been going on with intrusive thoughts. We just didn’t know that was what it was, so we wanted to let them know. It was a lot easier to tell them.

As far as friends, I told my best friend and he was very understanding, though I was nervous that he wouldn’t quite get it or understand, but I didn’t tell anyone else for quite a long time because I just was not ready for that yet. When I diagnosed was a very rough year because I had been bullied and picked on all year long my first year of high school, which led me to transfer to a new high school. That was a good change for me.
When I was first diagnosed I started doing ERP in a group with others that had just been diagnosed as well. It was just nice being around others that had been going through their own OCD journeys as well, and to know I wasn’t the only one going through this.
What has helped you the most in your recovery process?
ERP [exposure and response prevention], and medication have helped. But what I always come back to is the OCD community. I went to my first IOCDF conference in 2018 in Washington DC when I was going through a rough patch at the time.
I was very nervous to go, but my parents thought it could be very helpful for me, and was it ever! I went there knowing no one, and met so many people who just got me, and understood me.

The next year I went to the Austin IOCDF conference and was much more comfortable and that was the year I really started to make friends that I stay in contact with on a regular basis to this day via phone conversations, Zoom meetings, and social media.
Knowing I am not alone in this has helped me more than anything. I am just blown away with how loving, supportive, and caring the OCD community is. I think of it as my extended family now.
What do you wish people understood about OCD?
That OCD is a very stigmatized disorder and it is not just about wanting things clean or wanting things color coordinated. OCD comes in so many different forms. This is a disorder that is very debilitating and that is hard to live with, and when I see things such as shirts, etc. making fun of OCD it is hurtful.
If you could give just one piece of advice to someone with OCD, what would it be?
That you can live a very fulfilling, meaningful life even though you have OCD. There are so many resources, medications, people out there that can help you live that meaningful life. You are not alone in this fight.
August 30, 2023
Book Review: At Last Count
My last Q&A was with Claire Ross Dunn, the author of the novel At Last Count, and I’m back to talk about the book!
At Last Count was a fast read, but not in a light and fluffy way (although I love those books too!). Since the main character, Paisley, has obsessive-compulsive disorder (OCD), there is a heaviness to the story, and what kept me reading even when I felt a little heartbroken for her was my desire to know what the heck happened when she was a teenager: Why had she been living in the same dingy apartment since she turned 18, and how could she afford even that in a big city (Toronto) on a part-time salary?
Chapters alternate between the life of current-day (2007), 39-year-old Paisley and that of 13-year-old Paisley in 1981. Both timelines give readers an accurate portrayal of how OCD can manifest (Paisley’s obsessions are around a fear of fire and her compulsions involve checking and counting in series of eight) and how it can disrupt a person’s life. Paisley is smart, has her degree, and has a part-time job, but she has a hard time getting out of the house.
She did not need a relationship. She did not want people in her apartment where she might have to act normal when she wasn’t feeling normal, and most of all, she did not want to have to share her secrets.
At Last Count
I appreciated that although Paisley is nearly 40 her life isn’t together. It’s sad, but it’s real. Since At Last Count is fiction it’s not meant to reflect a perfect world in which Paisley gets a diagnosis as a child, sees a trained and knowledgeable therapist who guides her through exposure and response prevention (ERP), and goes on with her life armed with all the right tools. What it does do is show the reader how confusing her symptoms were to experience, how people who have no idea what OCD is are concerned about Paisley’s counting, and how she wasn’t diagnosed in childhood despite displaying the symptoms for years. Some of her solutions to dealing with her OCD and making it “better” are common but ineffective and downright harmful, showing readers what is a normal lack of knowledge of the disorder.
‘Will things get better if I count eight sets of eight? Will I prevent a fire if I touch each light switch and outlet eight times? Not likely. But I do it anyway.’
Paisley, At Last Count
Readers will feel for Paisley as she struggles—even if they don’t have OCD or understand much about it, the torment is palpable. At Last Count is a sweet, sad, sometimes scary, and somewhat mysterious novel about a woman with OCD, but it’s not just about OCD. For those of us with the disorder, that part is the cherry on top.
July 10, 2023
Author of At Last Count: Claire Ross Dunn
As varied as our OCD stories can be, it always amazes me when I relate with someone’s story as much as I have with that of today’s guest, Claire Ross Dunn. We both have a thing with the number eight, we both have obsessions around a fear of fire, and we both put our book drafts in a drawer for several years before we finally got them published. And I am so glad Claire wrote her book, At Last Count! (Stay tuned for a review in a few weeks.) Read more about Claire’s inspiration for the book, how she navigated OCD before resources were widely available, and how she’s doing now. Thank you, Claire!

You recently published your first book, At Last Count, a coming-of-age novel whose protagonist has OCD. What inspired you to write At Last Count?
I did not set out to write a book about OCD. I started a writers’ circle with two friends around 2005 to create a space where I could just write for pleasure. The world of film and television, which is where I predominantly make my living, can be quite high stress, and I was glad to find a space for writing just for the joy of it. I started writing a short story about an introvert who falls in love with a bookseller at a very famous bookstore in Toronto, that is now closed, called the Albert Britnell Book Shop. It was a classic bookstore with floor-to-ceiling wooden bookshelves with ladders, and very knowledgeable staff; a dreamy place. So I was working on this short story, and two arts council literature grant deadlines to write books came up. We challenged each other to submit, and I received both of them. Suddenly I realized I had to write a novel, even though I didn’t know how. That’s how At Last Count started.
It wasn’t until many drafts and two fiction writing courses later, after I had submitted to three publishers and had been very gently rejected, that I realized suddenly that I was writing a book about OCD, and about my own experience in my youth with OCD. So ultimately, even though I didn’t know it, I guess my own OCD was the inspiration. But it took a very roundabout course. I think I had to coax my own brain into it.
Writing a book (and getting it published, no less!) is no small feat. Writing a book about a disorder that caused you so much personal pain even more so. Can you tell us about the writing experience? Did you question your decision?
Did I question that decision? Absolutely—only about a hundred times. I felt tremendous levels of stress submitting the book to publishers. That would have been around 2012. I knew the book was good enough to submit, because I had worked with several editors and mentors, all of whom I trusted. And so I was surprised at the level of stress I was feeling, given how often I pitch to producers and broadcasters in my life in television. What was up with all the stress? I literally couldn’t breathe.

After all three publishers said no thank you, and they all were very kind about it—they liked the book, but it wasn’t right for them—I felt tremendous relief. It was in that moment that I suddenly realized I had written about my OCD experience. I had conceived a book that was entirely fictional about a woman and her complex love affair with a childhood nemesis, but I’d actually written it from this very true place of having suffered from this OCD as a young person. And I just wasn’t sure what to do with any of it.
On a practical level, I was afraid that people in TV would find out that I had struggled so much with this anxiety disorder as a youth. I was probably through the worst of it by my mid-20s, but I will admit that I still have shadows of it to this day. There are things I will and won’t do, things that I know to stay away from because they are triggers, and just a general higher level of anxiety than the regular person.
So when those three publishers said no thank you in 2012, I shoved the book in a drawer for eight years. I told myself that trying to publish a book was folly—I’ve read that the rate of people getting their book published lies somewhere between 1 and 2 percent, so the chances of it happening are really low. I told myself that I had a successful career in television, and didn’t need to publish a book.
I didn’t really think about the book again until 2020, when COVID struck. The Canada Council for the Arts came out with a $5,000 grant to digitally pivot any project artists had on deck—a brilliant way they were trying to sustain the artist community that had been so badly affected by the pandemic—so I decided to apply. I couldn’t think of anything I could do for $5,000 in television, but suddenly I had this brainwave: I could record an audiobook of At Last Count. That, I felt I could do for $5,000.
Even then, I thought: I don’t have to admit to anybody that the book is inspired by my own experience with OCD. It will just be a small COVID project, no one will know, and it will keep me artistically occupied during the pandemic. But as luck would have it, I hired a wonderful and very experienced editor, Alex Schultz, who I thought should kick the tires on the book before I hired actors and an audiobook director. And he loved the book so much, he offered to submit it to a publisher, Invisible Publishing. Of course I was overjoyed, but I was also suddenly plunged right back into the dilemma that I’d had before, which was that if a publisher were to like it and want it, I would likely have to talk about the OCD. So I crossed my fingers and toes hoping that that wouldn’t be the case, but right before Alex passed it to the publisher, he called me and said, “I have to ask you about the OCD. Is this your personal experience?” My knees literally shook during that phone call, even though Alex is as lovely as can be. I was just terrified to talk about it.

So for the first time in my life, I had to admit to someone I didn’t know very well that I had OCD. It was scary, but I got through it. I’m so glad I did. I had the same conversation with the publisher when they offered to publish it, and even though that was scary, too, my knees shook less. Each time I have the conversation, I get a bit more used to talking about it. Still, as we went through the pre-publication process, which takes about a year and a half, I started to wonder if I’d made the right choice. Of course I knew I had, on a very deep level, because there’s truly nothing more joyful for a writer than publishing a novel, and I adore my publishers.
What do you hope readers will walk away with after reading At Last Count? Do you think they’ll be surprised by the depiction of OCD in the book—at least if they don’t know much beyond the surface?
I hope readers will come away with a few different things.
One, an empathy about the internal experience of OCD. There is not one thing that is fun about it, to put it mildly. It’s a terrible, awful thing, something you wouldn’t wish on anybody. I struggled with it alone when I was young, because it was the 70s, and because there was no Internet where I could do research myself, or join an online organization, and I was an only child, and honestly, a good secret keeper. No one knew I was having trouble, and so I was terribly alone in it. I’ve had amazing responses from readers—both those who have struggled with OCD, and those who have known very little about it before reading the book. In fact, recently, the publisher has begun selling the book to high schools, which of course thrills me because it means the book gets exposed to two different sets of readers—adults, and teens—and I spoke about it to a conference of psychologists for a school board who were very happy to have good, fictional reading material available for their students that accurately depicts the internal experience of OCD.
The second thing I hope readers come away with is the notion that you don’t have to believe everything your brain tells you. OCD, to me, is a very talented trickster. It tells you things that sound like absolutes. It wants you to believe them to feed its engine. The more you give in to the rituals, the more believable and vital they seem. And it’s a moving target, so if you manage to get out of one set of compulsions, it looks for another to keep you in check. It took me a long time to figure out that those are just thoughts, not facts.
The last thing I hope readers come away with is the power in asking for help. In the book, Paisley finally gets help with her love interest Garnet, even though she’s kept her secret so long, and it’s just what she needed. As I mentioned before, I struggled with OCD in the ’70s and ’80s, when there was no internet, and it wasn’t possible to find resources online. There might have been an OCD organization somewhere, but if there was, I had no way of knowing about it. Now it’s so different.
During the pandemic, after I knew that the book was going to be published, I thought that I had better read up on OCD, because I had had the very strange experience of having struggled with it, at its worst, for probably 20 years, but knowing very little about it. I went online and found the IOCDF (the International OCD Foundation, based out of the US). They did an amazing job of pivoting during the pandemic, bringing so much of what they do online, in livestream interviews with knowledgeable guests, webinars, and virtual conferences. I had the remarkable experience of listening to others talk about OCD, both experts and those who struggle with it, and realizing that I was not alone. It was an epiphany for me: people were using the exact words that had come out of my mouth, the exact same thought patterns that I had struggled with. It was just shocking and revelatory, in that I finally realized how not alone I was.
What makes me happiest is that the book can be read on two levels—yes, to get a real picture of what having OCD is like—but also, it can be read purely for the story: this complex, layered, intense love affair between two people who manage to help each other out of a tough place. The book is uplifting (I won’t say more for fear of spoilers), but people who love a good page-turner romance can easily read the book for that alone. Much of the feedback I’ve received has been that while I wrote about something that is very hard, I also wrote a joyful book that has hope at the end. That seems to have been recognized as an achievement. And that was an important thing for me: to give people hope. Because I live a pretty great life. I am married to a prince of a husband, we’ve been married for 31 years, we have two wonderful children, and I have a good career, doing the thing I most love to do, which is writing. All of these things are possible, even for someone with OCD.
How long have you had OCD? Can you share some of your symptoms with us?
I figure it was since about the age of seven or eight or so. I can’t be sure, but I do remember certain points of my life when I was definitely struggling with it. It was worst until my mid 20s. And although I think there is no magic bullet for such a thing, my OCD really abated after I got together with my husband, Kirk, who is calm and kind and was a big stabilizer in my life. After Kirk proposed to me and we’d set a date for the wedding, I immediately found a therapist and said, I have a year and a half to get myself sorted. Ready, set, go. (Nothing like a concrete goal like a wedding to motivate you.) OCD was a big piece of what we worked on together.

My dominant OCD symptom was counting and checking. My number was eight (because this you could conveniently count on two hands, thumbs to the tip of each finger), and I counted lots of things eight times, over and over. I had a massive fear of fire, so I got into patterns when I was young, checking the stove, every light fixture and electrical outlet in the house eight times. When things were very bad, I would do the whole sequence of checks eight times. You can imagine, it was pretty time-consuming. Uncertainty about these things spun off into other areas, like false memory (I didn’t cook, but I’m worried the stove is on, so maybe I did cook and don’t remember?), and scrupulosity—needing to feel very clean about everything I do, dot the i’s, finish a task perfectly. And asking for reassurance or apologizing for the most simple things over and over. It’s exhausting and can trigger all sorts of feelings of self-loathing. Why can’t I beat these thought patterns? What’s wrong with me?
The other way OCD manifested was extreme feelings of responsibility and concern about the safety of others. This was a deep spiral and repetitive cycle of concern for me.
I still struggle with negative thought patterns, and a concern about people’s safety, but I live a very high-functioning life. I no longer count. I am never relegated to the house, unable to leave because of fear of fire. One of the really important concepts I learned from attending these IOCDF webinars was the notion of approximation. OCD tells us that every aspect of our lives must be perfect: I must be 110 percent sure I didn’t leave the stove on, and if I have to check it eight times, then that’s a good thing.
But where we want to get to is the idea that good enough is the gold standard. I can check the oven once before I leave the house, I know it’s off, and even if I doubt it, I can walk out the door and go to my appointment. OCD tells us that the more we check, the more clarity we’ll get, but instead it creates confusion, and we become less clear. And OCD is always happy to offer the solution: check again. It’s okay. You’ll feel better. It takes some training to believe that that feeling of imperfection is okay. And the more I practice living in that imperfection, the healthier I am.
Once you knew what you’d been experiencing was OCD, did you tell anyone—family, friends, strangers? How did they receive the information?
By the time the book published, I would say maybe five or six people all told knew that I had OCD. I honestly have no recollection of the earliest people I told. I don’t think I would have even had a term for it back then. So it must have been when I was much older that I realized what the diagnosis was. I remember seeing a book on psychology on my brother-in-law‘s shelf, and in it was a chapter on OCD with an OCD questionnaire, which I took standing there, trying to act all nonchalant as I read this book. And of course I passed with flying colors. So that was a lightbulb moment. But, for example, I didn’t tell my children until the book was about to be published. That was a big moment. And they were awesome about it. By that time they were both in their 20s. So they listened to my story and then said, you rock, Mum. You got through this hard thing. Amazing. And that time, my knees didn’t shake.
If you could offer just one piece of advice to someone with OCD, what would it be?
It would be that thing I spoke about above: you don’t have to believe everything your brain tells you. Thoughts aren’t necessarily facts. And if we can discern the difference, get evidence-based help by qualified professionals, and tell OCD that it has no place in our life, then we can get on with having our awesome, good-enough lives. Maybe we can’t get rid of OCD 100 percent. But we can tell it firmly that while it can come along for the ride, it doesn’t get to drive.
June 6, 2023
Balancing Multiple Diagnoses: Brooke Miller
Help me welcome Brooke Miller, who advocates for awareness of obsessive-compulsive disorder (OCD) and eating disorders, bipolar II, and panic disorder. Brooke has been through many trials and has a lot of wisdom to share, so read on for her story and how she balances it all. Thank you, Brooke!
Can you share a little of your background with us, including your experiences with OCD, an eating disorder, bipolar II, and panic disorder?
Well, buckle up because my mental health journey has been quite a ride!
 Shuffle Photography LLC
Shuffle Photography LLCLooking back, my first encounter with OCD behaviors happened when I was around 8 to 10 years old. Folding my dirty laundry before tossing it in the hamper became a must-do ritual to avoid any imagined disasters. As I grew older, my OCD manifested in various forms like contamination fears, perfectionism, harm obsessions, “just right” tendencies, and even magical thinking.
Throughout school and college, I had high achievements and appeared flawless on the outside, but inside, anxiety and stress were slowly eating away at me. It took a lot of courage to seek help for the first time, but unfortunately, my initial therapy experience wasn’t fruitful. Undeterred, I tried a couple more therapists who, although well-meaning, didn’t specialize in exposure response prevention (ERP), which is crucial for OCD recovery.
In 2012, after becoming a mom, my OCD took on a whole new dimension, making it nearly unmanageable. It was a wake-up call, and I finally reached out to a local mental health community outreach program. They connected me with a therapist who is an absolute rock star in OCD and ERP. With his guidance, I learned what true OCD treatment and recovery entailed, and together, we dove into the hard work.
Feeling optimistic, I thought I could handle things on my own and took a break from therapy. Little did I know, a relentless form of OCD called “Pure O” struck me, but I kept it hidden, resulting in missed opportunities for treatment. Eventually, I returned to my therapist’s care as I experienced my first panic attack fueled by a brand new OCD subtype—relationship OCD. Intrusive thoughts and images flooded my mind, causing immense shame and convincing me that I was a cheater.
My self-loathing spiraled, leading to significant weight loss, anorexia nervosa, and a dangerous cycle of punishment. It was a turning point when I finally accepted that I needed help. I underwent an intensive treatment program, followed by outpatient therapy with a dedicated treatment team for both OCD and my eating disorder. It was a journey of ups and downs, relapses and recoveries, but I made slow but steady progress.
Just when I thought things were finally falling into place, life threw another curveball. In 2022, I experienced a manic episode and was diagnosed with bipolar II. Balancing the intensity of my OCD exposures while ensuring stability became my new challenge. With the right medication and ongoing therapy, I began to regain my equilibrium and made remarkable strides in my OCD recovery. It felt like I was finally getting a handle on things.
But the surprises weren’t over yet. Fall of 2022 brought yet another diagnosis: Panic disorder. Frequent and intense panic attacks became a daily struggle. For weeks, my treatment team and I worked tirelessly to manage them. Thankfully, a combination of medication and interoceptive exposures began to bring them under control.
And here we are today! I’m doing really well, managing all my mental health disorders and making progress in my recovery every single day. It hasn’t been easy, but my journey has taught me resilience, perseverance, and the incredible strength of the human spirit.
Remember, my story is just one among millions. We all face unique challenges, but we also share the capacity to overcome and thrive. Let’s continue to support each other, break the stigma, and remind ourselves that mental health is a journey worth taking.
You share a lot of your recovery journey on your blog, Smashing Stigmas. What inspired you to start writing about your experiences?
I firmly believe that those with lived experience are the true experts when it comes to mental health. Unless we’ve walked in someone’s shoes, it’s difficult to grasp the challenges of living with a mental health disorder. That’s why I am dedicated to amplifying the conversation about mental health in our society. Through my blog, Smashing Stigmas, I openly share my personal journey of struggles and triumphs on the path to recovery. My goal is to instill hope in others, showing them that with the right support and resources, they too can experience healing. No one should feel alone in their struggles, and by shedding light on mental health, we can create a world where these experiences are openly discussed and embraced. It’s my passion to use my own recovery journey to uplift and inspire others on their own paths toward wellness.
You’re also an IOCDF Advocate! Why did you decide to join this program? What do you hope to achieve in your role?
I am beyond thrilled and deeply honored to be an IOCDF Advocate! My heart’s desire is to make a meaningful impact by raising awareness, shattering stigmas, and ensuring everyone has access to vital mental health resources. Through sharing my personal journey, I aim to empower individuals grappling with OCD and related disorders, offering them hope and reminding them they are not alone. With this role, I aspire to educate the community, ignite passion for advocacy, and foster a world where mental health is embraced and supported by all.
How do your different diagnoses affect each other, if at all? Has it been a challenge to balance different treatment methods and make sure one doesn’t have a negative impact on another?
I was genuinely amazed to discover how interconnected my different diagnoses are and how they can influence one another. Strikingly, the treatment methods for my OCD, anorexia, bipolar II, and panic disorder showed remarkable similarities, which brought a glimmer of hope to my journey towards recovery. One invaluable approach that played a pivotal role was ERP, a technique employed to tackle my OCD, anorexia, and panic disorder. Through this method, I gradually confronted my fears, dismantled obsessive patterns, and reclaimed control over my life.
Medications have also played a crucial role in my healing process. To balance the serotonin levels in my brain, I take a selective serotonin reuptake inhibitor (SSRI), which has been immensely helpful. Additionally, I have utilized a mood stabilizer to minimize the intensity of depressive and manic episodes associated with bipolar II. It’s been a delicate balance, requiring time and perseverance, but finding the right combination has been instrumental in managing my mental health.
In the past, managing one condition often meant the other would spiral out of control. It felt like a relentless game of whack-a-mole, where as soon as I focused on one aspect, the other would worsen. However, the challenges I faced have been mitigated by the unwavering support of my incredible treatment team. Their collaborative efforts and dedication have been nothing short of a lifeline. My therapist, dietitian, psychiatrist, and primary care provider have worked in harmony, ensuring that I receive the best possible holistic care. I am eternally grateful to them for their unwavering support and guidance on this arduous journey.
Today, I stand as a testament to the power of perseverance and the importance of compassionate care. While it hasn’t been an easy road, the similarities in treatment methods and the commitment of my exceptional team have filled me with optimism. I have learned that even in the face of multiple diagnoses, there is hope for recovery and the opportunity to live a fulfilling life. With the right support, dedication, and a touch of resilience, I believe in the possibility of a brighter future.
What do you consider the biggest misconception about OCD? What about eating disorders?
Ah, let’s break those stigmas and misconceptions once and for all! When it comes to OCD, I believe that the biggest misconception is often the belief that it’s just a quirky personality trait or something enjoyable. Please, let me be clear: OCD is a mental health disorder that can have a profound impact on a person’s life. It’s not a choice, and it’s definitely not something anyone desires or asks for.
Similarly, with eating disorders, there’s a prevalent misconception that they are simply a matter of willpower or a deliberate choice. Nothing could be further from the truth! Eating disorders are serious mental and physical illnesses. In fact, they are known to be one of the most lethal mental health conditions. We must recognize the severity and urgency surrounding these disorders.
It’s time to join forces and challenge these misconceptions head-on. We need to educate ourselves and others, spreading awareness that OCD and eating disorders are not character flaws or choices. They are real, complex, and often devastating conditions that deserve our understanding and support.
Let’s come together as a community to reduce the stigmas that surround these mental health disorders. By sharing accurate information, supporting those affected, and fostering empathy, we can create a more compassionate world where individuals with OCD and eating disorders can feel safe, heard, and understood!
If you could give just one piece of advice to someone with OCD, what would it be?
Oh goodness, only one piece of advice… I’ll try!
First and foremost, I want them to know that they are not alone in this journey. OCD can make you feel isolated and trapped, but there is hope and support out there for you.
My biggest piece of advice would be to seek the right treatment. With the right support and therapy, you can regain control over your life and create a path that aligns with your true values, rather than those dictated by OCD.
Remember, treatment for OCD is not a quick fix, but it is absolutely worth it. Find a therapist who specializes in OCD and ERP, as this evidence-based approach has been shown to be highly effective. Building a strong therapeutic relationship with someone who truly understands your struggles can make a world of difference.
Don’t underestimate the power of support from others who have walked a similar path. Seek out support groups, online communities, or even reach out to mental health organizations specializing in OCD. Connecting with others who truly understand can provide immense comfort and a sense of belonging.
Above all, be kind to yourself. Recovery is a journey, and there will be ups and downs along the way. Embrace your progress, celebrate your victories, and show yourself compassion during the challenging moments. You are stronger than you know, and you have the capacity to reclaim your life from the clutches of OCD!



