Nancy Kay's Blog
April 20, 2026
One Client Who Taught Me An Invaluable Lesson
I was a young veterinarian when I met Martha, a kind, soft-spoken woman devoted to Murphy, her nine-month-old cocker spaniel. Martha told me that three other veterinarians had already run a myriad of tests, but nothing was found to be amiss. According to Martha, the other veterinarians thought Murphy was normal, and she was a hypochondriac.
 Photo by Tanya Barrow on Unsplash
Photo by Tanya Barrow on UnsplashMartha confessed that were no clear-cut symptoms. Yet, she was certain that something was troubling her beloved dog. His appetite and activity level at home were normal, and there had been no vomiting, diarrhea, coughing, or sneezing. It was while Murphy was on his daily walks that something felt off to Martha. He was a bit less exuberant than normal.
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
I examined Murphy from teeth to toenails, hoping for the clue that would help guide the diagnostic process. I reviewed all the laboratory test results and X-rays previously generated. Still nothing. Was Martha truly a hypochondriac? After listening to her and observing her body language, my intuition told me otherwise. I admired Martha’s calm perseverance. After being turned away three times, here she was in her ongoing efforts to be an effective medical advocate for her dog.
Though Murphy did not have a heart murmur, based on the possible change in his energy level, I suggested an echocardiogram—an ultrasound examination of his heart.
Lo-and-behold, this study revealed the abnormality responsible for Martha’s concern. Murphy had a birth defect called a patent ductus arteriosus (PDA). The ductus is a normal blood vessel in the developing fetus that closes off shortly after birth. In some puppies, this ductus remains open, causing abnormal blood flow that can ultimately result in heart failure.
In most PDA’s, the abnormal flow moves from the left side of the heart to the right side and causes a loud heart murmur, which Murphy did not have. This typical PDA can be corrected, and the dog goes on to live a normal life.
Murphy’s PDA was atypical—the abnormal blood flow moved from the right side of the heart to the left. This “reverse direction” does not cause a heart murmur, the reason the three veterinarians before me had been stumped.
Sadly, there wasn’t a feasible way to correct this reverse-direction PDA, meaning Murphy’s symptoms would progress.
When I explained the diagnosis to Martha, she cried. She told me her tears were a combination of sadness and relief that her concerns had finally been validated. She was grateful that the search for a diagnosis was over and she now knew what to expect.
Martha and Murphy enjoyed another 18 months of good quality time together. When his symptoms intensified and he was euthanized, Martha sent a note letting me know and thanking me for having believed in her.
For decades (and I won’t specify how many!) I’ve remained profoundly indebted to Martha for teaching me a valuable lesson. She taught me that no one knows my patients better than my clients, and it pays to trust their instincts, gut feelings, and intuitions about their pets. When they sense something is wrong, their hunches deserve my attention and investigation.
I’ve thought about Martha and Murphy hundreds of times while evaluating animals with ill-defined or subtle symptoms. Martha’s perseverance was truly inspirational.
Have you ever had a hunch that something was wrong with your pet even though there were no obvious symptoms? If so, how did things pan out?
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
drnancykay.com
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
April 13, 2026
Photos of Kids and Dogs: Adorable or Alarming?
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
Take a look at the photos below. Cute kids with cute dogs, right? What’s not to love? Now take a closer look. See any reason for concern?
Image number one
I think this dog’s eyes express apprehension/concern. I’ll bet his heart rate is elevated.
Notice the girl’s hands. Many dogs detest having their feet handled.
Look at how close this little girl’s face is to this dog’s mouth. If he loses his patience and bites rather than removing himself from the situation, the result could be devastating.
Image number two
Does this dog look happy and comfortable in this situation? I think not.
Again, see where this child’s face is in relation to the dog’s mouth?
Image number three
Yes, it’s unlikely that a puppy, a Labrador pup to boot, is gonna care what’s happening here. But messing with any dog of any age while they’re eating is 100% disrespectful to the dog.
Serious bite wounds are often a result of resource guarding, and food is a resource many dogs take very seriously.
Image number four
Climbing on a dog like this is the epitome of disrespect.
This Labrador may not care much, but the dog certainly doesn’t look happy in this photo.
Image number five
Based on this dog’s uncomfortable expression, I sense he’s thinking, “Please don’t come any closer.”
Once again, notice the proximity of the dog’s mouth to the child’s face.
Image number six
Now, this is an image that I love! The dog appears content and is with this child by choice. The kiddo is petting him in a very respectful manner.
A Story About MaxMax was a favorite patient of mine—a huge, gentle St. Bernard. When he came in to see me, he was accompanied by his owner Beth and her two young kiddos who had no qualms about treating Max like a beanbag chair. They flopped all over him. Yet Max never complained.
Twice, I explained to Beth that I was concerned about how the kids were treating Max. She was convinced Max enjoyed it as much as the kids.
Imagine my shock when Beth scheduled an appointment for Max to be euthanized. The poor dog finally snapped and caused severe damage to the face of one o f the children. This was heartbreaking for everyone involved. Thankfully, Beth allowed me to re-home Max to a household without young children.
It’s not a dog’s job to know how to interact with kids. It’s your job to teach your kids how to interact with dogs!Please share your thoughts on these photos. Do you think I’m being overly cautious? Any words of wisdom about the combination of dogs and children?
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
drnancykay.com
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
April 6, 2026
Wacky Tales of Whacking Tails
Wagging tails are great, right? They convey so much happiness. But sometimes, wagging tails can be problematic. Watch this video of a tail that operates like a constant metronome. Imagine if we could harvest all that wag as an energy resource!
Problematic Tail WaggingEver observed wagging tails upend flower vases and knock over beverages? People living with these waggers must “tail-proof” their homes!
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
Ever been slapped across your thigh by a tail that stings like a whip? And the more you react, the more the dog wags? Ouch!
Happy Tail SyndromeVeterinarians commonly deal with tail tip trauma, aka “happy tail syndrome.” It’s caused by repeated whacking of the tail against a firm surface such as a wall, door, or refrigerator. The blood loss isn’t a significant issue and rarely is the wound very painful.
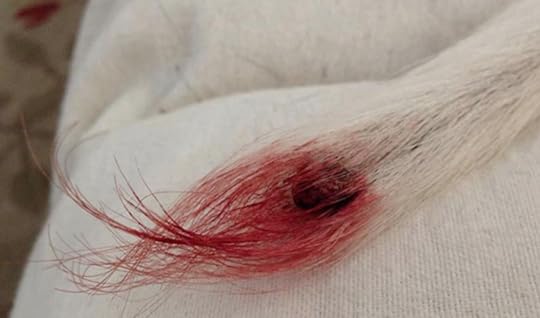 Happy Tail Syndrome
Happy Tail SyndromeNo big deal, right? Wrong! A seemingly simple problem is anything but.
How do you prevent the tail of a happy dog from becoming a living paintbrush, spattering red around your home, creating a personalized CSI crime scene? Immobilizing a dog’s tail is pretty much impossible as is keeping a bandage in place.
How do you prevent the dog from licking and chewing at the tail tip long enough to let it heal?
Once the sore heals, how do you prevent it from recurring?
Treatment OptionsThere are several things worth trying:
Stop the bleeding with 5-10 minutes of pressure over the wound.
Use an Elizabethan collar to keep the dog’s mouth away from the tail tip (must be a very large collar).
Try to prevent wagging against hard surfaces. (Happen to have a padded room?)
Bandage the tail. Keep in mind that a bandage covering just the tip is likely to slide right off. Consider running it up the length of the tail.
Secure a protective cover, such as an empty syringe case, over the bandage.
Sedate the dog to lessen the amount of tail wagging.
Extreme as it may sound, amputation of the end of the tail is the treatment of choice if other tactics fail to work or if the problem is recurrent. The tail revision (partial amputation) need not be as extreme as a Rottweiler or Australian shepherd look. Rather, the post-op appearance can be more the length of an Airedale or Vizsla tail—short enough to prevent it from banging against hard surfaces.
Have you ever had a dog who wagged its way into a problem?
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
drnancykay.com
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
March 30, 2026
Recent Results From the Dog Aging Project
The Dog Aging Project is a monumental research undertaking that has enrolled more than 50,000 dogs. The purpose of the project is to determine the impact of genetics, lifestyle, and environment on canine longevity.
 Research results
Research resultsThe Dog Aging Project has already completed several studies. Undoubtedly, there will be more to come. Here’s a handful to get you started.
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
2025: Risk Factors for Gastric Dilatation-VolvulusGastric dilatation-volvulus (GDV), aka, gastric torsion, is a horrific disease in which the stomach twists on itself. Picture a fanny pack. One of the straps represents the esophagus that carries food from the mouth to the stomach. The other strap represents the duodenum that transports food out of the stomach. Now, imagine holding both straps and twirling the pack on itself (crimping the straps). Not only does this obstruct outflow from the stomach, it crimps off important blood vessels.
Without emergency surgery (and sometimes even with it) the patient succumbs.
Research from the Dog Aging Project determined that dogs with increased risk for GDV were purebred, were male, had a body weight > 40 kg (88 pounds), had a low body condition score, and were Poodles/Poodle mixes. There was no increased risk associated with fearful or anxious behavior, neuter status, age at the time of neutering, diet type, or the number of meals fed per day.
2025: Nutritional Completeness of Home-Prepared DietsThe composition of 1,726 home-prepared (homemade) diets varied widely. Ingredients included: meats, vegetables, fruits, grains, nuts, seeds, and oils. Only 6% of these diets were nutritionally complete according to the Association of American Feed Control Officials adult dog maintenance standards.
For those of you who are strongly against commercially prepared dog food, remember, I’m just the messenger!
2025: Diet Type and Owner Reported Health IssuesResearchers evaluated the diets of 27,478 dogs. Home-prepared diets were associated with higher odds of gastrointestinal, liver, and kidney diseases compared to dogs eating an extruded diet (kibble). A commercial raw diet was associated with higher odds of respiratory disease compared to an extruded diet.
Remember, I’m just the messenger!
2025: Biomarkers of MortalityResearchers discovered that dogs and humans share some of the same biomarkers (a measurable substances in the body) that are predictors of mortality. The researchers concluded that, given their relatively short lifespan, dogs may be an extremely valuable translational model to understand the underlying molecular causes and consequences of age-related human mortality.
2022: Association Between Physical Activity and Cognitive Dysfunction in Older DogsCanine cognitive syndrome is widely recognized as the doggie version of dementia. Researchers showed that, just as in people, dogs’ physical activity is associated with better cognitive outcomes.
2021: Canine Cognitive Dysfunction Scores Correlate with the Amyloid Levels Within the BrainThere appear to be parallels between Canine Cognitive Dysfunction (CCD) and Alzheimer’s Disease (AD) in people. Both are associated with excess accumulation of the protein amyloid within the brain tissue. In this study, dogs with more severe CCD symptoms had higher concentrations of amyloid within certain areas of their brains (evaluated post-mortem).
TRIAD Study (in progress)I recently wrote about the anti-aging drug, rapamycin and the Triad Study (Test of Rapamycin in Aging Dogs). Can’t wait to see these results.
Want to enroll your dog in the Dog Aging Project and/or the TRIAD study? The only prerequisite is that you have a reasonably accurate sense of when your dog was born. Click here to learn how to enroll.
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
drnancykay.com
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
March 23, 2026
A Testimonial About Second Opinions
In 2024, I wrote a blog post called, A Second Opinion Is Always Okay. I received the following letter pertaining to this topic in which the moral of the story is a favorite line of mine:
“What’s more important, your dog’s health or your veterinarian’s feelings?”
Hello Dr Kay,
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
I want to thank you for your book. I really believe it is the reason that my boy Morgan is still with me today. My husband gave me Speaking for Spot about three months ago as a birthday present and I read it cover to cover.
Morgan had been sick on and off since he was a year old. When Morgan began getting sick again two weeks ago my vet kept putting me off telling me that he was a retriever and he probably just ate something that upset him and he would get over it like he had done in the past.
I knew better so I reread the chapter on asking for a second opinion and when he continued not to listen I had a meeting with him and asked for a referral to a specialist in internal medicine. I have to tell you my heart was pounding like crazy, I felt like I was betraying my vet. He gave me Morgan’s file but sadly not the referral. He felt I should find another vet as he felt I had lost confidence in him.
I got an appointment on my own for the next day and on the way there my boy had a seizure, at least I think that’s what it was. I was terrified he was not going to survive until we got to the clinic. Needless to say he was very ill, but he survived and may come home tomorrow. The diagnosis was Addison’s disease.
So thank you for writing the book. I am convinced that without it Morgan would have died while I blindly followed my vets advice.
Thank you so much,
Brenda
High five to Brenda’s husband who gave the gift of Speaking for Spot!
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
drnancykay.com
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
March 19, 2026
Deadline Extended To Take Action to Improve the Lives of Breeding Dogs in Puppy Mills
The USDA just extended their deadline to April 20th to submit comments about the care and well being of breeding dogs in puppy mills. Please, please provide your suggestions/feedback. Here is the link to do so. You do not need to respond to every prompt. The more voices supporting improved conditions for these dogs, the better!

Thank you!
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
drnancykay.com
March 16, 2026
Five Takeaways From Facilitating a Pet Loss Support Group
For ten years I was privileged to facilitate a weekly pet loss support group. Participants ran the gamut in terms of age, wealth, and experience with the loss of loved ones.
 Photo by Jackie Best on Unsplash
Photo by Jackie Best on UnsplashHere are five takeaways from my experience:
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
1. GuiltGuilt is prevalent among people who have lost a pet. There were so many reasons some of which included:
If only I’d noticed he was sick sooner.
If only I hadn’t been out of town.
If only I hadn’t said “yes” to that surgery.
I did what my vet said I should do, but I think it was too soon.
I think we waited too long and he suffered.
I could have done more.
One distraught participant threw a ball for her dog that rolled into the street. You can imagine what happened. Talk about guilt!
As a facilitator, I always tried to direct the guilt-ridden person’s focus back to their intentions—always good, never bad.
2. The magnitude of the hurtMany people voiced shame and confusion when explaining that the loss of their pet felt more devastating than the loss of a close relative, such as a parent. I think the discrepancy in feelings has to do with the unconditional, nonjudgmental love our pets provide and the fact that decision-making about euthanasia is limited (for the most part) to veterinary medicine.
3. The euthanasia processI often heard regrets about not being with their pet during the euthanasia process. Only occasionally were people regretful about having been present because things did not go smoothly or as expected.
The moral of the story—if possible, opt to be present with your beloved pet.
4. The reentry processPart of the reason my grief group was so popular was that many folks had difficulty finding meaningful support within their normal lives. Well meaning friends and relatives had empathy, but only for a finite period. They reported hearing things such as:
You can always get another dog/cat.
It’s been three weeks. Shouldn’t you be feeling better?
Oh c’mon. He was only a pet.
When grieving, it’s important to seek out others who are patient and willing to understand your experience.
5. Sharing stories and photos of the lost petWhen this happened in my support group, there were always smiles and “aww’s” around the room. Always a lovely respite from the grief in the room.
Has the loss of a pet ever brought you to your knees? Were you able to find the support you needed?
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
drnancykay.com
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
March 9, 2026
Tracheal Collapse in Dogs
“My dog won’t stop coughing, and I’m not getting any sleep!” What veterinarian hasn’t heard this complaint? Several disorders can cause coughing in dogs. One at the top of the list, particularly in smaller breeds, is called tracheal collapse (aka, collapsing trachea).
 Photo by charlesdeluvio on UnsplashThe normal trachea
Photo by charlesdeluvio on UnsplashThe normal tracheaThe trachea, also known as the windpipe, transports air from the nose and mouth down into the lungs, then back out again. It’s made up of rings of cartilage, aligned side by side to maintain a smooth cylindrical shape that creates minimal resistance to airflow. Visually speaking, the trachea looks like a corrugated culvert pipe that you’d find at a building supply store.
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.

The entrance to the trachea is the larynx, a cartilage structure that opens during breathing and closes during swallowing. This clever design prevents inhalation of food material into the lungs (aspiration pneumonia).
The inside lining of the trachea contains millions of cilia, fine little hairs that trap inhaled particulate matter. Using a coordinated sweeping action, the cilia then transport these particles, often embedded in mucous, up to the throat for disposal by coughing or swallowing.
Tracheal collapseImagine the normal, semi-rigid, “O” shaped tracheal cylinder collapsing in on itself, resulting in a “C” shaped internal lumen. This is tracheal collapse. It’s problematic, not only because of impaired airflow in and out of the lungs, but also in terms of removal of inhaled debris.
The actual collapse is usually a dynamic process—more pronounced during inhalation or exhalation, depending on which portion of the trachea is affected.
Dogs at riskAn inherited defect in the tracheal cartilage is thought to be the major player in the development of tracheal collapse. Small breed dogs are the “poster children” for this disease, particularly Yorkshire terriers, pugs, Pomeranians, poodles, and Chihuahuas. Middle-aged and older dogs are more commonly affected. Overweight dogs and those who live in households are at greater risk.
SymptomsTracheal collapse invariably causes coughing that’s often described as sounding like a “goose honk.” However, the cause of a cough cannot be diagnosed based on the sound of the cough, and tracheal collapse is no exception.
Tracheal collapse coughing often worsens in response to excitement, activity, or exercise (when air is moving more vigorously through the trachea) and when exposed to smog, smoke, increased temperature, humidity, and airway allergies.
The cough may be persistent or intermittent. There may be audible wheezing, particularly during inspiration. At its worst, tracheal collapse causes labored breathing, purple or blue-colored tongue and gums caused by oxygen deprivation, and syncopal (fainting) episodes.
Making the diagnosisThe first step is to take X-rays (neck and chest) of the trachea. Given that the collapse may be associated with just inhalation or exhalation, a plain X-ray can miss the diagnosis. For this reason, fluoroscopy (an X-ray but shot in movie mode) is the ideal diagnostic tool.
Tracheoscopy (viewing the inside of the trachea with an endoscope) may be recommended to confirm the diagnosis and gather samples to rule out an underlying respiratory tract infection.
Management toolsWhile there is no cure for tracheal collapse, there are multiple management strategies for minimizing the coughing and maintaining a good quality of life. Realistically, it’s often difficult to eradicate the coughing altogether.
Lifestyle changesWeight loss can make a positive difference for obese dogs with tracheal collapse.
It’s a no-brainer that a dog with tracheal collapse and cigarette smoke exposure has a lot to gain by lifestyle changes made by their beloved humans.
Avoidance of known environmental factors that precipitate coughing (heat, humidity, smog, etc.) can make a big difference.
Replacing a neck collar with a chest harness eliminates external pressure on the trachea.
MedicationsIt’s almost always necessary to rely on medications when managing dogs with significant tracheal collapse symptoms. For some dogs, only short-term or intermittent use is needed. Other dogs thrive only with long-term, if not lifelong, medication.
Antitussive therapy (cough suppression): For dogs with a collapsing trachea, coughing tends to beget more and more coughing. And once a vicious coughing cycle begins, it can be difficult to interrupt. Often, more than one antitussive medication is tried to find just the right recipe to quiet the cough.
Control of secondary inflammation: Anti-inflammatory medications are used to control the inflammation associated with tracheal collapse. Until the inflammation settles down, it can be difficult to control the coughing.
Treatment of secondary bacterial infections: Antibiotics are commonly used to treat possible infection.
Sedation and/or reduction of anxiety: Severely affected dogs may suffer from chronically interrupted sleep and/or anxiety induced by constant coughing and labored breathing.
Oxygen therapyIn severe cases of tracheal collapse, a day or two spent in an oxygen cage may help the dog turn a corner. Such oxygen therapy requires access to a 24-hour hospital and round-the-clock supervision.
Tracheal stentsWhen medical treatment fails to restore a good quality of life, placement of a tracheal stent might be considered. The stent, made of a metallic alloy, is placed within the area of tracheal collapse. Once deployed, the stent expands to support the tracheal walls. While this procedure can make a positive difference in severe cases of tracheal collapse, not every dog is an ideal candidate. There can be problems associated with anesthesia and complications caused by the stent.
SurgerySurgical techniques involve placement of support rings around the outside trachea. The goal is to provide structural support. This is an aggressive procedure that can be fraught with complications. With the increasing popularity of tracheal stents, this type of surgery has, for the most part, fallen by the wayside.
PrognosisThe prognosis for dogs with tracheal collapse varies from excellent to awful. The outcome depends on the degree of collapse, which portion(s) of the trachea is involved, and the dog’s individual response to medication.
Veterinary specialistsIf your dog develops tracheal collapse, a veterinary internal medicine specialist might just become your dog’s new best friend. The more finesse and experience a veterinarian has using medications to treat tracheal collapse, the greater the likelihood of a positive outcome, particularly in severely affected dogs.
Have you had a dog with tracheal collapse? If so, what worked and what didn’t?
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
March 2, 2026
The Dog Auction Mindset
I had the eye-opening experience of spending a day at Southwest Auction Service where dogs are auctioned off like livestock. I described my observations in a previous post.

Those in attendance were mostly puppy millers— there to buy or sell animals—along with a smattering of folks from dog rescue organizations.
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
Below is an email I just received from Southwest Auction Service (yes, I joined their email list). Such a blatant representation of the inhumanity of puppy mills!
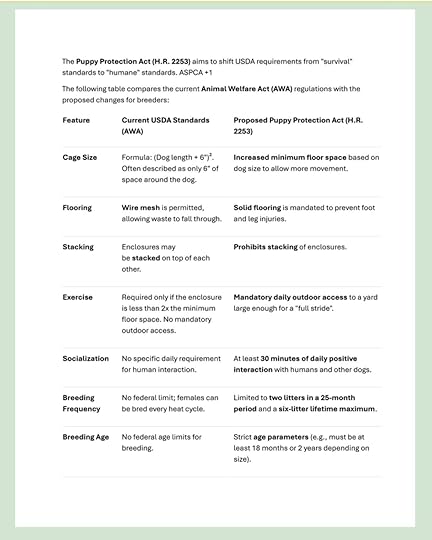


Each time I look at this chart, I feel shock and outrage! How about you?
Two Things We Can DoThe United States Department of Agriculture (USDA) is the regulatory body for livestock in this country, which sadly includes puppy mills. A quick and simple thing you can do is sign this Humane World for Animals petition asking the USDA to support more humane standards in puppy mills.
Here’s a second opportunity to make a difference. Between now and March 19th, the USDA is soliciting public comments regarding two puppy mill standards:
The care of breeding female dogs, including cage size, number and frequency of litters, nutritional needs, and veterinary care.
Socialization and exercise needs of dogs living in puppy mills.

This is an excellent opportunity for the public to weigh in on improving conditions for dogs serving life sentences in puppy mills. I encourage you to participate (okay to answer only the questions you like). Please share this with your veterinarian as their voices need to be heard.
You can find a description of current USDA puppy mill regulations here. Remember to submit your comments by March 19th.
LET’S DO THIS!!
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
DrNancyKay.com
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
February 23, 2026
Temperament Testing in Dogs
Let’s say you want to adopt a puppy from a litter of ten. How will you decide which one to bring home? Based on gender, color, or markings? Based on how sleepy or active or smitten with you they appear during your brief visit? How can you confidently choose which one will be the right fit for you and your household?
 Photo by Laura Roberts on UnsplashTemperament Testing
Photo by Laura Roberts on UnsplashTemperament TestingThe best way to predict the adult behavior of young puppies is through temperament testing. This assessment is best performed on 7-week-old pups (give or take a little bit) by someone with temperament testing experience.
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
Pups are exposed to various situations and are scored based on their confidence level, social behavior, desire for play, and reactions to play stimuli, prey stimuli, loud noise, and separation.
Here’s a fun video of temperament testing on a litter of beagle puppies.
Looking for a chill family dog, a long-distance running partner, a hunting dog? Results of temperament testing can help guide you.
Temperament Testing Based on SalivaA study published earlier this month on adult dogs documented that the amount of cortisol (a stress hormone) and serotonin (a feel-good hormone) in their saliva correlated with behavior patterns.
Concentrations of salivary cortisol and serotonin were measured in 24 dogs before and after standardized temperament testing. Findings showed that the dogs with higher stress reactivity, based on temperament testing, had higher cortisol levels. Serotonin levels were increased in those with greater emotional regulation (stability).
This study has a very small sample size (24 dogs) and I look forward to results of more studies to validate these findings. I wonder if, some day, such testing might be practical enough to allow shelters to better match dogs with their forever homes.
Have you had experience with temperament testing? If so, did you (do you) find it helpful? I’d love for all my dog trainer/behaviorist readers to chime in.
Best wishes to you and your four-legged family members for abundant good health,
Dr. Nancy
DrNancyKay.com
Speaking for Spot - Dr. Nancy Kay is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.



